Featured Answer: What happens at a dental implant consultation?
At Innova Smiles, a dental implant consultation is a thorough, educational session lasting roughly 60 to 90 minutes. We begin by reviewing your medical history and performing a clinical exam of your mouth. We capture a precise 3D CBCT scan to evaluate your jawbone density and nerve pathways. Finally, Dr. Fatima discusses all viable replacement options, expected timelines, and provides a transparent, itemized breakdown of costs, including insurance benefits and financing options. You leave with a printed treatment plan and complete clarity about next steps.
Introduction: Taking the First Step Toward Confidence
Deciding to replace missing teeth or stabilize loose dentures with implant-supported options is a life-changing choice. The American Academy of Implant Dentistry reports that more than 5 million implants are placed annually in the United States, and that number continues to grow as outcomes improve and costs become more accessible. Implants represent a permanent investment in your oral health, allowing you to eat, speak, and smile with absolute confidence.
However, because implant placement involves a surgical procedure and careful long-term planning, the process can feel intimidating for patients who have never been through it. If you live in Marlborough, MA, or the surrounding communities of Northborough, Southborough, or Hudson, the team at Innova Smiles aims to demystify this process entirely. It all begins with the implant consultation.
This guide walks through every step of your first implant visit -- what we check, what technology we use, and what the costs look like. By the end, you will know what to expect and what to ask.
Who Is a Candidate for Dental Implants?
Before diving into the consultation process, it helps to understand who qualifies as a candidate for dental implants. Dental implants are appropriate for most adults who:
- Are missing one or more teeth, or have teeth that are failing and need extraction
- Have sufficient jawbone density to support the implant (or are willing to undergo bone grafting to build it up)
- Do not have uncontrolled systemic conditions that impair healing
- Are committed to maintaining good oral hygiene after placement
Age alone is rarely a disqualifying factor. We have placed implants successfully in patients in their 70s and 80s at Innova Smiles. The determining factors are bone quality, overall health, and healing capacity -- not the number on your driver's license.
Patients who wear dentures and are frustrated with slipping, adhesive pastes, and dietary restrictions are also excellent candidates. Implant-supported overdentures (such as All-on-4) can stabilize a full arch of replacement teeth on as few as four strategically placed implants.
Step 1: Delving into Your Medical and Dental History
Your safety and the long-term success of the implant are our highest priorities. Before we even look inside your mouth, we must have a full understanding of your overall health.
Why Your Medical History Matters
According to the American Academy of Implant Dentistry (AAID), a dental implant relies on your body's ability to heal and fuse bone to the titanium post -- a biological process called osseointegration. First described by Swedish orthopedic surgeon Per-Ingvar Branemark in the 1960s, osseointegration is the foundation of modern implant dentistry. Certain medical conditions can impact this healing process.
During your consultation, we will meticulously review:
- Current Medications: We are specifically looking for blood thinners (warfarin, Eliquis, Plavix), bisphosphonates used for osteoporosis (Fosamax, Boniva, Reclast), and immunosuppressants. Bisphosphonates are of particular concern because long-term use can, in rare cases, impair jawbone healing. A 2021 position paper from the American Dental Association concluded that the risk of medication-related osteonecrosis of the jaw (MRONJ) is low for oral bisphosphonate users but must be evaluated on a case-by-case basis. Dr. Fatima will discuss your specific risk profile.
- Systemic Health Conditions: Uncontrolled diabetes (HbA1c above 8 percent) slows wound healing and increases the risk of implant failure. A 2019 meta-analysis in the Clinical Oral Implants Research journal found that patients with well-controlled diabetes (HbA1c below 7 percent) had implant survival rates comparable to non-diabetic patients. Autoimmune disorders, recent chemotherapy or radiation to the head and neck, and severe osteoporosis also require careful evaluation.
- Lifestyle Habits: Research in the Journal of Dental Research confirms that smoking drastically impedes blood flow to the gums and jawbone, raising the risk of implant failure by two to three times. Nicotine constricts blood vessels, reducing oxygen delivery to healing tissue precisely when it is most needed. We will discuss cessation strategies and, if appropriate, may recommend postponing surgery until you have been tobacco-free for a minimum period.
- Previous Dental History: We want to understand why the teeth were lost in the first place. Teeth lost to advanced periodontal disease indicate a different risk profile than teeth lost to trauma. We also review any history of dental anxiety and discuss gentle care options if needed.
What to Bring to Your Consultation
- Your dental insurance card and a photo ID
- A current list of all medications and supplements
- Any recent dental X-rays or records from a previous provider (we can request digital transfers)
- A list of questions -- we encourage patients to write them down ahead of time
Step 2: The Clinical Examination
Next, Dr. Ambereen Fatima will perform a thorough physical examination of your mouth.
Assessing the Foundation
Placing an implant requires a healthy oral environment. A titanium post integrated into infected or compromised tissue will not succeed no matter how skilled the surgeon. Dr. Fatima will evaluate:
- Gum Health: The American Academy of Periodontology (AAP) stresses that active periodontal (gum) disease must be treated before an implant can be safely placed. If we detect pocketing, bleeding, or clinical attachment loss, we will develop a gum treatment plan that stabilizes your periodontal health before beginning the implant process. This preliminary step may add a few weeks to your overall timeline, but it protects your investment.
- Surrounding Teeth: We check the health and stability of the teeth adjacent to the missing tooth gap. Decay, fractures, or root infections in neighboring teeth can compromise the implant site and may need to be addressed first.
- Bite Alignment: We evaluate how your upper and lower teeth meet. A heavily unbalanced bite can place excessive, destructive lateral forces on a new implant crown, increasing the risk of mechanical failure. If bite correction is needed, Dr. Fatima will incorporate it into the treatment plan.
- Soft Tissue Quality: The thickness and quality of the gum tissue around the implant site affect both healing and the final aesthetic result, especially in the "smile zone" (front teeth). Thin, fragile tissue may require a connective tissue graft to create a natural-looking gum contour around the restoration.
- Existing Restorations: We examine any crowns, bridges, or partial dentures that may interact with the planned implant. Sometimes an implant eliminates the need for an existing bridge, simplifying your overall dental situation.
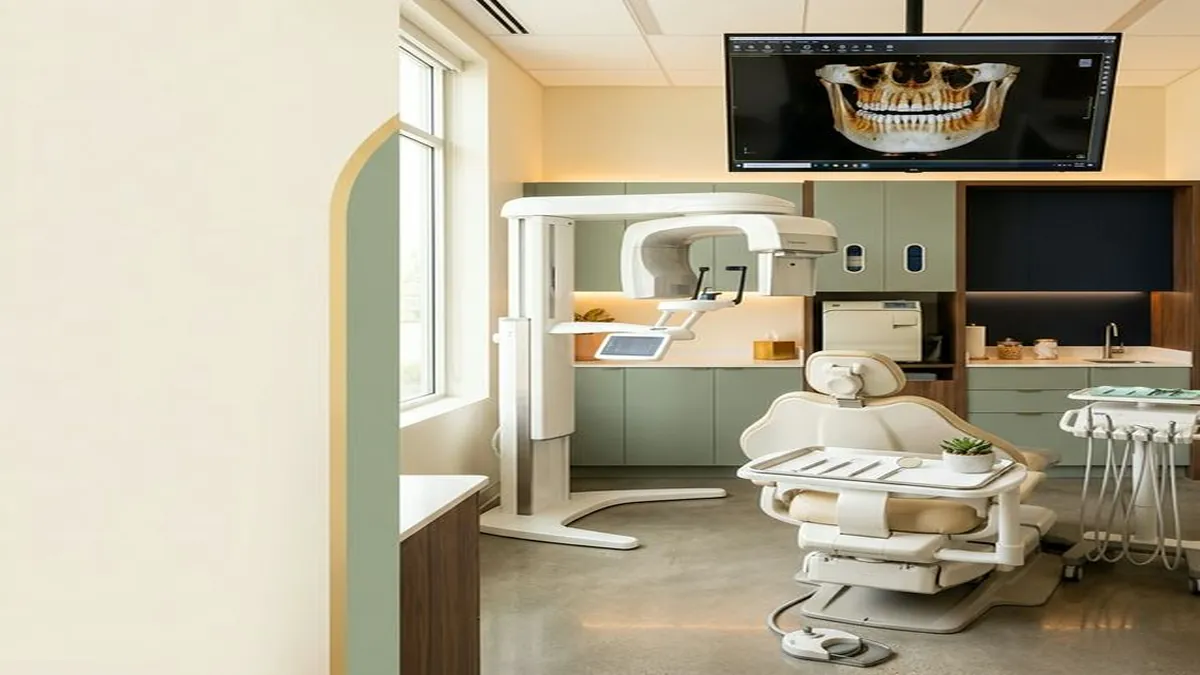
Step 3: Advanced 3D Imaging (CBCT)
The most critical phase of modern dental implant planning occurs using advanced digital imaging.
Standard 2D dental X-rays are excellent for finding cavities, but they are insufficient for planning implant surgery. A periapical or panoramic X-ray shows a flat, two-dimensional shadow of a three-dimensional structure. Bone width, the proximity of the mandibular nerve canal, and the exact topography of the sinus floor are invisible on these flat images. At Innova Smiles in Marlborough, we use an in-house CBCT (Cone Beam Computed Tomography) scanner to eliminate this diagnostic blind spot.
The Power of 3D Precision
A CBCT scan takes only 15 to 20 seconds but provides a highly detailed, three-dimensional model of your entire facial structure. The radiation dose is significantly lower than a medical CT scan -- roughly equivalent to a standard panoramic X-ray, according to the American Academy of Oral and Maxillofacial Radiology. This allows Dr. Fatima to:
- Measure Bone Volume Precisely: We can evaluate exactly how tall, wide, and dense your jawbone is at the proposed implant site, measured in millimeters. If the bone has atrophied (shrunk) due to tooth loss -- and bone resorption begins within weeks of extraction -- we can proactively plan for a bone graft or sinus lift to rebuild the foundation. The CBCT data tells us exactly how much bone augmentation is needed and where.
- Map Vital Structures: The 3D view allows us to pinpoint the exact location of the inferior alveolar nerve canal in the lower jaw, the mental foramen (where the nerve exits the bone), and the sinus cavities in the upper jaw. A 2020 study in the International Journal of Oral and Maxillofacial Implants found that CBCT-guided implant planning reduced the rate of nerve-related complications by more than 90 percent compared to freehand placement from 2D imaging alone.
- Assess Bone Density: Different regions of the jaw have different bone densities. The posterior maxilla (upper back jaw) is typically the least dense, which affects implant selection and healing protocols. Dr. Fatima factors density into the surgical plan, sometimes selecting wider-diameter implants or recommending a longer osseointegration period in softer bone.
- Virtual Surgery: Using specialized implant planning software, Dr. Fatima virtually "places" the implant on the 3D model, adjusting angulation, depth, and position until the optimal configuration is achieved for both surgical success and the final aesthetic crown. In many cases, this virtual plan is used to fabricate a surgical guide -- a 3D-printed template that seats over your teeth and guides the drill to the exact planned position during surgery.
Surgical Guides: From Virtual Plan to Precise Execution
Guided implant surgery is one of the most significant advances in implant dentistry over the past decade. The 3D-printed surgical guide transfers the digital plan directly to the surgical field, eliminating the hand-eye estimation that characterized traditional freehand placement. A 2022 systematic review in the Journal of Clinical Medicine found that guided surgery achieved a mean deviation of less than 1.2 mm at the implant tip compared to the planned position -- a level of precision that protects nerves, maximizes bone engagement, and ensures ideal prosthetic angulation.
Step 4: Discussing Options and the Treatment Plan
Armed with clinical data and 3D imaging, Dr. Fatima will sit down with you to discuss the findings in clear, understandable language.
We believe in collaborative care. Dr. Fatima will explain whether you are a direct candidate for immediate placement, or if preliminary procedures (like extractions, bone grafting, or periodontal treatment) are required. She will also discuss the type of implant restoration best suited to your situation:
- Single-Tooth Implant and Crown: Replaces one missing tooth with a standalone implant and custom crown. This is the most common implant procedure and preserves the adjacent teeth without alteration.
- Implant-Supported Bridge: Replaces three or more consecutive missing teeth using two implants as anchors for a bridge, rather than placing an individual implant for each missing tooth. This reduces surgical sites and cost while still providing a fixed, permanent restoration.
- Implant-Supported Overdenture: For patients missing most or all teeth, four to six implants can anchor a full-arch prosthesis that snaps securely into place. The All-on-4 approach is a popular option for patients currently wearing removable dentures who want a fixed, non-removable solution.
Your fellowship advantage: It is important to know who is designing your treatment. Dr. Fatima has achieved prestigious Fellowship status in the International Congress of Oral Implantologists (FICOI) and the American Academy of Implant Prosthodontics (FAAIP). Her advanced training means your implant is planned "prosthetically driven" -- meaning we start by designing the perfect final tooth in its ideal position, then engineer the surgical placement backward to support that result precisely. This approach, endorsed by a 2021 consensus statement from the International Team for Implantology (ITI), produces better aesthetics, better function, and higher long-term survival rates than surgery-first planning.
Step 5: Understanding the Timeline
Implant dentistry is rarely a "same-day" process (though some patients do qualify for same-day dental implants), and the final result is worth the patience. Here is a realistic breakdown of the dental implant planning timeline:
Phase 1: Preliminary Procedures (if needed)
- Extraction of failing teeth: 1 visit, with 8 to 12 weeks of healing before implant placement (in some cases, the implant can be placed immediately at the time of extraction)
- Bone grafting: 1 visit for the graft, followed by 3 to 6 months of healing while new bone matures. Socket preservation grafts (placed at the time of extraction) typically heal in 3 to 4 months; larger block grafts or sinus lifts may require 5 to 6 months.
- Periodontal treatment: Scaling and root planing, possible surgical periodontal therapy; timeline varies based on severity
Phase 2: Implant Placement Surgery
The surgical appointment itself typically takes 1 to 2 hours per implant under local anesthesia (with available). You go home the same day.
Phase 3: Osseointegration
The implant must fuse with the jawbone before it can support a permanent restoration. Osseointegration typically requires 3 to 6 months, depending on bone quality and location. During this period, you may wear a temporary restoration -- a flipper, temporary bridge, or healing cap -- so you are never without teeth.
A 2018 prospective study in Clinical Implant Dentistry and Related Research found that allowing adequate osseointegration time before loading the implant resulted in 10-year survival rates above 96 percent. Rushing this phase to save a few weeks is not worth the risk.
Phase 4: Abutment and Final Crown
Once osseointegration is confirmed (Dr. Fatima verifies integration clinically and radiographically), we place the abutment (the connector piece) and take impressions for your custom crown. The final crown is typically delivered 2 to 3 weeks later. For most patients, the total process from consultation to final crown spans 4 to 9 months.
Step 6: Financial Transparency
You will meet with our treatment coordinator, who will provide a written, itemized breakdown of the proposed treatment. There are no hidden fees. We outline the cost of imaging, surgical placement, bone grafting (if applicable), abutments, and the final restoration.
Typical Implant Costs at Innova Smiles
| Component | Approximate Cost |
|---|---|
| CBCT scan | $150 to $350 |
| Single implant (surgical placement) | $1,800 to $2,500 |
| Abutment | $500 to $800 |
| Custom implant crown | $1,200 to $1,800 |
| Total (single implant, no grafting) | $3,500 to $5,000 |
| Bone graft (socket preservation) | $400 to $800 |
| Sinus lift | $1,500 to $3,000 |
| All-on-4 full arch | $20,000 to $30,000 |
We will actively help you maximize your benefits:
- Insurance Navigation: We will check your specific dental plan. Many PPOs now cover portions of the implant process, such as the final crown (often classified as a major restorative service at 50 percent coverage) or preliminary extractions. Some medical insurance plans also cover bone grafting when medically necessary.
- Flexible Financing: We work with CareCredit and Cherry to offer 0-percent-interest payment plans for qualified patients, allowing you to break the investment into manageable monthly payments.
- Membership Value: For patients without traditional insurance, our Innova In-House Membership Plan provides significant saving tiers on implant procedures. Membership patients also receive discounted imaging and exams throughout the treatment process.
- HSA and FSA: Dental implants are an eligible expense for Health Savings Accounts and Flexible Spending Accounts. If your employer offers these pre-tax benefit accounts, they can reduce your effective out-of-pocket cost by 20 to 35 percent depending on your tax bracket.
What Happens After the Consultation
Most patients leave their implant consultation what to expect session feeling significantly more confident than when they arrived. Here is what happens next:
- Review at home: Take your printed treatment plan home and review it with your family or partner. We encourage questions and are happy to schedule a follow-up phone call to address anything that comes up.
- Insurance verification: Our billing team submits a pre-authorization to your insurance carrier and provides you with a detailed benefits breakdown, typically within 5 to 7 business days.
- Schedule surgery: Once you are ready to proceed, we schedule your surgical appointment. If preliminary procedures are needed, those are scheduled first.
- Pre-surgical instructions: You will receive written guidelines covering medications to avoid, eating and drinking restrictions (if is used), and what to arrange for the day of surgery (a driver, soft foods at home, ice packs).
Frequently Asked Questions About Dental Implant Consultations
How long does the consultation appointment take? Plan for 60 to 90 minutes. This includes the medical history review, clinical exam, CBCT scan, discussion of findings, and the financial breakdown. We never rush this appointment.
Is the consultation painful? Not at all. The clinical exam is gentle, and the CBCT scan is comfortable -- you simply stand still for 15 seconds while the scanner rotates around your head. No needles, no drilling, no anesthesia.
Do I need a referral from my general dentist? No referral is needed. Patients from across MetroWest -- Westborough, Shrewsbury, Framingham, and beyond -- schedule directly with our office.
What if I have been told I do not have enough bone for implants? Bone insufficiency is common after long-term tooth loss, but it is rarely a permanent disqualifier. Modern bone grafting techniques -- including guided bone regeneration, block grafts, and sinus lifts -- can rebuild the jawbone to support implants in the vast majority of cases. Dr. Fatima's CBCT analysis will determine exactly what augmentation is needed and whether implants are feasible for your situation.
Can I get a dental implant if I have gum disease? Active gum disease must be treated and stabilized first. Placing an implant in an infected environment leads to peri-implantitis (implant gum disease) and a high risk of early failure. The good news is that modern periodontal treatment is highly effective, and most patients can proceed to implants within a few months of completing their gum therapy.
Ready to Rebuild Your Smile?
Your implant consultation at Innova Smiles is a thorough experience designed to give you all the information you need to make the best health decision for your future.
- Explore our comprehensive approach: Dental Implants in Marlborough
- Learn about how we make care affordable: Insurance & Financing
- Need immediate help? Emergency Dental Care
Start your treatment with clarity and confidence. Call Innova Smiles today at (508) 481-0110 or request a consultation online to map out the future of your smile.
Related Articles
- Day-by-Day Dental Implant Recovery Timeline
- Dental Implant Cost Guide for Massachusetts
- Why FICOI & FAAIP Credentials Matter for Implants
- What to Expect During Dental Implant Surgery
- All-on-4 Dental Implants: Full Mouth Restoration Guide
- Dental Implant Materials: Titanium vs. Zirconia
- Does Dental Insurance Cover Implants? A Massachusetts Guide