Featured Answer: Who qualifies for implants?
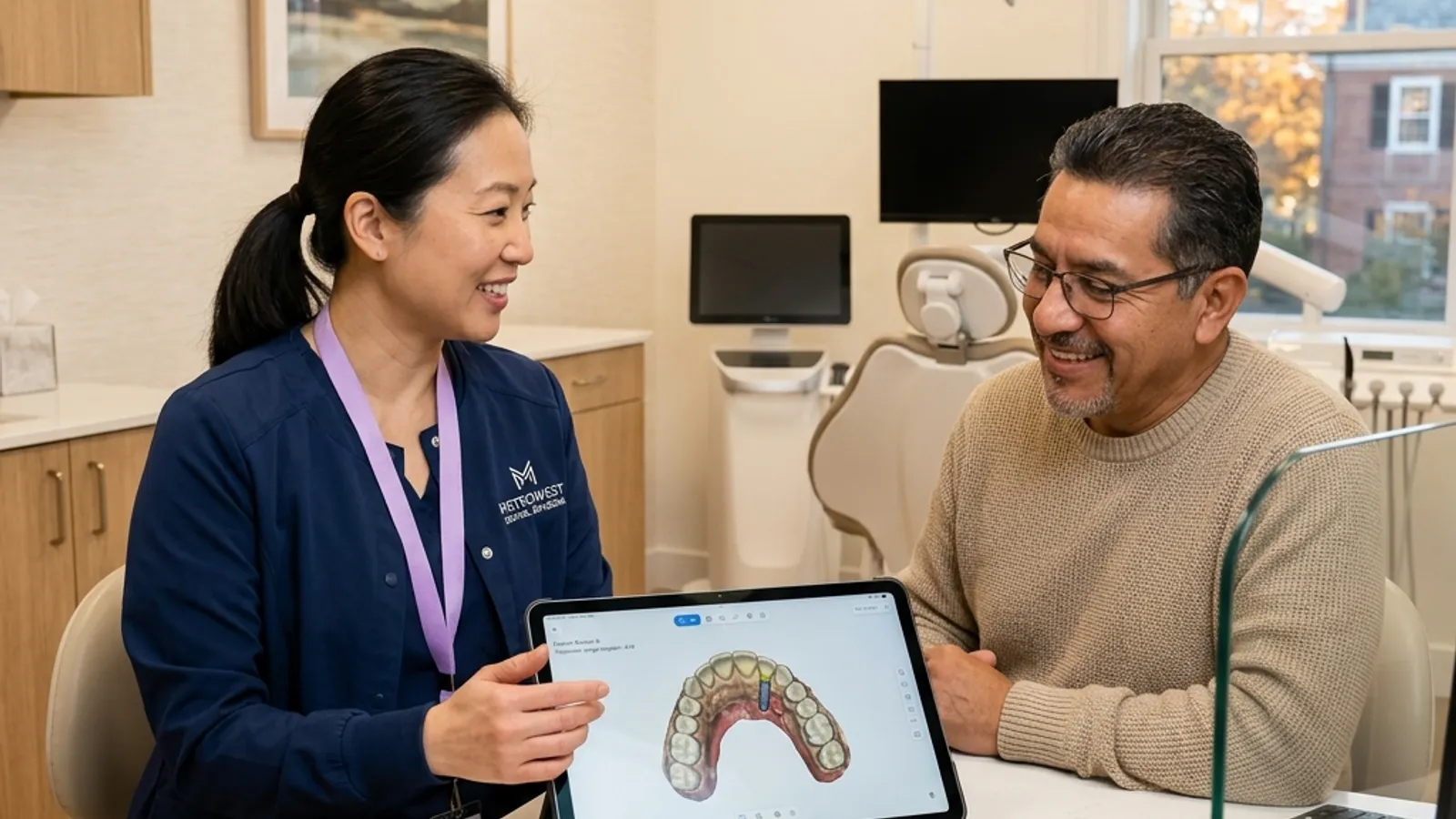
Healthy gums, adequate bone (or grafting potential), and controlled medical conditions are key. A consultation with 3D imaging confirms suitability and maps your plan.
If you are considering dental implants in Marlborough, MA or the surrounding MetroWest communities, the first question on your mind is probably: "Am I actually a candidate?" The answer, for the vast majority of adults, is yes, but the path to that answer requires a thorough evaluation. At Innova Smiles, Dr. Ambereen Fatima (FICOI, FAAIP) evaluates every patient individually using advanced 3D CBCT imaging and a comprehensive medical review to determine the safest, most predictable path forward.
The Comprehensive Candidacy Checklist
Before we get into the details of each factor, here is a high-level checklist of what Dr. Fatima evaluates during your implant consultation:
- Jawbone volume and density: Is there enough bone to anchor the implant, or is grafting needed?
- Gum health: Is active periodontal disease present? If so, it must be treated first.
- Overall health status: Are there medical conditions that affect healing?
- Medications: Do any current medications interfere with bone integration or surgical healing?
- Smoking status: Tobacco use significantly impacts success rates.
- Bruxism: Teeth grinding or clenching can overload implant restorations.
- Age and jaw development: Jaw growth must be complete before implant placement.
- Oral hygiene commitment: Long-term implant success depends on consistent home care.
- Realistic expectations: Implants are excellent, but they require the same care as natural teeth.
Most patients who come to our Marlborough office concerned about candidacy are pleasantly surprised to learn that modern techniques, including bone grafting, sinus lifts, and guided surgical protocols, have dramatically expanded who can receive implants. The question is rarely "can you get implants?" and more often "what preparatory steps are needed?"
Bone Density and Volume: The Foundation of Every Implant
Bone is the foundation of every successful implant. A titanium implant post must be surrounded by a minimum quantity and quality of bone to achieve osseointegration, the biological process where living bone cells grow directly onto the implant surface, locking it permanently in place.
The National Institute of Dental and Craniofacial Research (NIDCR) notes that after a tooth is lost, the surrounding jawbone begins to resorb. This process is most aggressive in the first 6 to 12 months, the Clinical Oral Implants Research journal published a 2015 study showing that the alveolar ridge can lose 25 percent of its width within the first year after extraction, and up to 40 percent within three years. The longer a tooth has been missing, the more bone has likely been lost.
How We Assess Your Bone
During your consultation, a 3D CBCT (cone beam computed tomography) scan reveals the exact height, width, and density of available bone in three dimensions. Unlike traditional 2D X-rays, CBCT imaging shows:
- Bone height: The distance from the ridge crest to critical structures like the inferior alveolar nerve (in the lower jaw) or the maxillary sinus floor (in the upper jaw). Standard implants require a minimum of 8 to 10 mm of vertical bone.
- Bone width: The thickness of the ridge from buccal (cheek side) to lingual (tongue side). A minimum of 6 mm is typically needed to accommodate a standard 4 mm diameter implant with at least 1 mm of bone on each side.
- Bone density: Classified on the Misch scale from D1 (very dense cortical bone) to D4 (very soft, porous trabecular bone). D1 and D2 bone provides the strongest primary stability. D3 bone is common in the posterior maxilla and is treatable with modified surgical protocols. D4 bone may require longer healing times or undersized osteotomy techniques to achieve adequate stability.
When Bone Is Insufficient
If your CBCT scan reveals insufficient bone, it does not mean implants are off the table. Bone augmentation procedures include:
- Socket preservation grafting: Performed at the time of extraction to maintain ridge volume. If you are planning to have a tooth extracted, ask about simultaneous socket grafting, it prevents the bone loss that would otherwise occur and typically adds only $300 to $600 to the extraction cost.
- Ridge augmentation: Bone graft material (human donor bone, bovine bone, or synthetic hydroxyapatite) is placed on the deficient ridge and covered with a collagen membrane. Healing takes four to six months before implant placement.
- Sinus lift: For upper back teeth where the maxillary sinus has expanded into the space where bone should be, Dr. Fatima elevates the sinus membrane and places graft material underneath. This creates the vertical bone height needed for implants in the posterior maxilla.
- Block grafting: For severe defects, a block of bone (usually harvested from the chin or ramus of the lower jaw) is secured to the deficient site with screws and allowed to integrate before implant placement.
Many patients from Hudson, Northborough, and other nearby MetroWest towns are surprised to learn that even after years of tooth loss, grafting can still make implants possible. A 2024 study in Clinical Oral Implants Research found that grafted bone sites achieve implant success rates comparable to native bone (94.6 percent vs. 96.1 percent at five years) when proper healing time is allowed.
How Implant Success Rates Compare
The American Academy of Implant Dentistry (AAID) reports that dental implants have an overall success rate exceeding 95 percent over a 10-year period. A 2019 systematic review published in the Journal of Dental Research analyzed data from over 10,000 implants and found a 10-year survival rate of 96.4 percent. When placed by an experienced clinician using guided surgical protocols and 3D imaging, success rates can approach 98 percent.
Factors that influence long-term success include:
| Factor | Impact on Success Rate |
|---|---|
| Bone quality and quantity | Higher density = stronger initial stability |
| Smoking status | Smokers: 85–90% vs. non-smokers: 95–98% |
| Diabetes (HbA1c) | Well-controlled (<7%): normal rates. Uncontrolled (>8%): increased failure |
| Oral hygiene | Good hygiene: 97%+. Poor hygiene: significantly higher peri-implantitis risk |
| Bruxism | Without night guard: 2x higher complication rate |
| Clinician experience | Higher-volume practices report better outcomes |
At Innova Smiles, Dr. Fatima's advanced FICOI (Fellow of the International Congress of Oral Implantologists) and FAAIP (Fellow of the American Academy of Implant Prosthodontics) training ensures that each implant is planned with 3D guided surgery and placed with the highest precision.
Medical Conditions and Implant Candidacy
Most adults in good general health are candidates for dental implants. However, certain conditions require careful evaluation and, in some cases, coordination with your physician. Here is what the evidence says about each major condition:
Diabetes
Diabetes is one of the most-studied conditions relative to implant outcomes. Elevated blood sugar impairs neutrophil function (your body's first-line immune cells), slows wound healing, and increases susceptibility to infection. A 2016 meta-analysis in the Journal of Dental Research found that patients with uncontrolled diabetes (HbA1c above 8 percent) had implant failure rates approximately 2.5 times higher than non-diabetic patients.
However, and this is the important part, patients with well-managed diabetes (HbA1c below 7 percent) showed implant success rates that were statistically indistinguishable from non-diabetic patients. If your diabetes is controlled through medication, diet, and monitoring, you are very likely a good candidate. Dr. Fatima may request a recent HbA1c lab result before scheduling surgery.
Osteoporosis
Osteoporosis reduces bone mineral density throughout the skeleton, including the jaws. However, the relationship between osteoporosis and implant failure is weaker than many patients expect. A 2020 systematic review in the International Journal of Oral and Maxillofacial Implants found no statistically significant difference in implant survival between osteoporotic and non-osteoporotic patients.
The more relevant concern is bisphosphonate medication. Drugs like alendronate (Fosamax), risedronate (Actonel), and zoledronic acid (Reclast) can, in rare cases, cause medication-related osteonecrosis of the jaw (MRONJ), a condition where jawbone exposed during surgery fails to heal. The risk is dose-dependent: patients on low-dose oral bisphosphonates for fewer than four years have a very low risk (estimated at less than 0.1 percent), while patients on high-dose IV bisphosphonates for cancer treatment have a meaningfully higher risk. Dr. Fatima evaluates your specific medication history, dosage, and duration to determine the safest timing for implant surgery.
Autoimmune Conditions
Rheumatoid arthritis, lupus, Sjogren's syndrome, and other autoimmune conditions, and more importantly, the immunosuppressive medications used to treat them (methotrexate, prednisone, biologics like Humira), can affect surgical healing. The impact varies significantly based on the specific medication, dosage, and disease activity. Dr. Fatima coordinates directly with your rheumatologist or prescribing physician to assess risk and, if needed, time the surgery during a period of stable disease control.
Heart Conditions and Blood Thinners
Anticoagulant therapy (warfarin, Eliquis, Xarelto, Plavix) does not disqualify you from implant surgery. Current guidelines from the American Heart Association recommend that most patients continue their anticoagulant medications through minor oral surgical procedures, as the risk of stopping the medication (stroke, pulmonary embolism) outweighs the risk of surgical bleeding. Dr. Fatima uses local hemostatic measures (oxidized cellulose, collagen plugs, precise suturing) to control bleeding during the procedure.
If you have a prosthetic heart valve or a history of endocarditis, prophylactic antibiotics are prescribed before the procedure per AHA guidelines.
Active Cancer Treatment
Radiation therapy to the head and neck area reduces blood supply to the irradiated bone, significantly increasing the risk of osteoradionecrosis (bone death) after surgery. The International Journal of Radiation Oncology recommends waiting at least 12 months after completion of radiation therapy before placing implants in irradiated bone, and some clinicians prefer a longer interval. Hyperbaric oxygen therapy (HBO) may be recommended to improve healing potential in irradiated bone.
Chemotherapy temporarily suppresses the immune system and impairs platelet function. Implant surgery is typically postponed until after chemotherapy is completed and blood counts have returned to normal ranges. Dr. Fatima works with your oncologist to determine the safest timeline.
Other Conditions
- Uncontrolled hypertension: Blood pressure should be stable before elective surgery. Readings above 180/110 require medical management before proceeding.
- Liver disease: Advanced liver disease affects clotting factor production and may require special surgical planning.
- HIV/AIDS: Patients with well-controlled HIV (adequate CD4 counts and suppressed viral load) have implant success rates comparable to HIV-negative patients, per a 2018 study in Clinical Oral Implants Research.
Age Considerations: No Upper Limit
According to the AAID, there is no upper age limit for dental implants. Patients in their 70s, 80s, and even 90s routinely receive implants with excellent outcomes, provided their overall health supports minor outpatient surgery. Age alone is never a disqualifier, functional status and medical health are what matter.
A 2021 study in the Journal of Prosthodontic Research specifically examined implant outcomes in patients over 80 and found a 5-year survival rate of 94.7 percent, only marginally lower than the general population rate. The authors concluded that "advanced age per se should not be considered a contraindication for implant therapy."
For older patients, the quality-of-life benefits are often even more dramatic. Patients who transition from poorly fitting dentures to implant-supported prosthetics frequently report significant improvements in nutrition (ability to eat a wider variety of foods), speech clarity, social confidence, and overall well-being.
For younger patients: Implants are typically placed after jaw growth is complete, usually around age 18 for females and 20 to 21 for males, though individual variation exists. Adolescents who lose a tooth to sports injury or trauma often use a temporary solution (a removable flipper or a bonded pontic) until skeletal maturity is confirmed with a hand-wrist X-ray or lateral cephalometric analysis. Placing an implant in a still-growing jaw can result in the implant becoming submerged as surrounding bone continues to develop, leading to a cosmetically unacceptable result.
The Impact of Smoking on Implant Success
Smoking deserves its own section because it is the single largest modifiable risk factor for implant failure. Research published in the Journal of Dental Research confirms that smokers experience implant failure rates two to three times higher than non-smokers.
The mechanisms are well understood:
- Vasoconstriction: Nicotine constricts blood vessels, reducing blood flow to the surgical site. Adequate blood supply is essential for osseointegration and wound healing.
- Impaired immune response: Smoking suppresses neutrophil and macrophage function, reducing the body's ability to fight infection at the surgical site.
- Increased peri-implantitis risk: Smokers have higher rates of peri-implantitis (infection around the implant), which is the leading cause of late implant failure. A 2019 study in Clinical Oral Implants Research found that smokers were 3.6 times more likely to develop peri-implantitis than non-smokers.
- Delayed bone remodeling: Nicotine inhibits osteoblast activity (the cells that build new bone), directly impairing the osseointegration process.
The good news: Patients who quit smoking before and after surgery see dramatically better outcomes. A protocol of smoking cessation at least two weeks before surgery and eight weeks after surgery (or ideally, permanent cessation) brings implant success rates much closer to non-smoker levels. Vaping and e-cigarettes are not a safe alternative, they still deliver nicotine, which causes the same vascular and healing impairments. If you smoke and are considering implants, talk to your physician about cessation support before your implant consultation.
Bruxism: Grinding and Clenching
If you grind or clench your teeth, a condition called bruxism, it does not disqualify you from implants, but it must be managed. Bruxism generates nocturnal forces up to 250 psi, far exceeding normal chewing forces. These forces are transmitted directly through the implant crown to the bone interface and can cause:
- Fracture of the implant crown or abutment
- Loosening of the abutment screw
- Crestal bone loss around the implant
- In extreme cases, fracture of the implant body itself
The solution is a custom night guard worn every night after the implant crown is placed. Dr. Fatima fabricates a hard acrylic guard that distributes clenching forces across all teeth, protecting both the implant and your natural teeth. This is a non-negotiable part of the treatment plan for any patient with a history of bruxism.
The Consultation Process at Innova Smiles: Step by Step
Your candidacy evaluation at our Marlborough office is thorough, educational, and takes approximately one hour. Here is exactly what happens:
Step 1: Medical and Dental History Review (15 minutes)
We discuss your complete medical history, current medications, allergies, and any previous dental work. If you have conditions that require coordination with another physician (diabetes, osteoporosis on bisphosphonates, heart conditions), we may contact your doctor before proceeding with surgery.
Step 2: Clinical Examination (15 minutes)
Dr. Fatima evaluates your gum health (probing depths, bleeding points, tissue quality), bite alignment, the condition of adjacent and opposing teeth, and the anatomy of the edentulous (toothless) site. If active periodontal disease is present, it must be treated and stabilized before implant placement, placing an implant in a mouth with uncontrolled gum disease is a recipe for failure.
Step 3: 3D CBCT Imaging (10 minutes)
A cone beam CT scan is taken in our office, taking about 15 seconds. While a CBCT scan delivers a higher radiation dose than a single panoramic X-ray—typically 3 to 4 times higher depending on field of view—the 3D imaging is essential for precise implant planning and is well within safe limits for diagnostic imaging. The resulting 3D dataset provides a complete map of bone volume, bone density, nerve pathways (the inferior alveolar nerve and mental foramen), sinus proximity, and the position of adjacent tooth roots. Dr. Fatima reviews this scan with you on-screen, pointing out the specific anatomy that will guide your implant placement.
Step 4: Treatment Planning Discussion (20 minutes)
Dr. Fatima presents your options based on the clinical and radiographic findings. This includes:
- Whether implants are indicated (single implant, multiple implants, implant-supported bridge, or full-mouth restoration)
- Whether preparatory procedures (bone grafting, sinus lift, gum tissue augmentation) are needed
- Expected timeline from start to final crown, learn more about the dental implant recovery timeline
- A written cost estimate with a line-item breakdown
- Insurance coverage details (our team verifies your benefits before the appointment)
- Financing options through CareCredit and Sunbit for patients who prefer to spread payments
Use our implant cost calculator to explore pricing before your visit.
The consultation is entirely pressure-free. You leave with a complete understanding of your options, the expected investment, and a clear path forward, whether that means scheduling surgery or addressing preparatory steps first.
What If I Have Been Missing Teeth for Years?
This is one of the most common concerns we hear from patients, particularly those who have worn dentures for a decade or more and assumed that their bone had deteriorated beyond the point of implant treatment. While prolonged tooth loss does lead to bone resorption, modern grafting techniques can rebuild the jaw to support implants in the vast majority of cases.
Dr. Fatima has placed implants for patients who have been edentulous for over a decade, using guided bone regeneration and sinus lift procedures to restore adequate volume. In some cases, shorter implants (6 to 8 mm rather than the standard 10 to 13 mm) or zygomatic implants (anchored in the cheekbone rather than the maxillary alveolar bone) can be used to avoid extensive grafting altogether.
The key is a thorough evaluation with 3D imaging to determine exactly how much bone is available and what supplemental procedures, if any, are needed. Do not let years of tooth loss discourage you from exploring your options.
Preparing for Your Candidacy Evaluation
To make the most of your consultation appointment at Innova Smiles, bring:
- A list of current medications, including dosages, over-the-counter supplements, and any recent changes
- Recent medical records, particularly if you have diabetes (recent HbA1c), osteoporosis (bone density scan results), or are on blood thinners (recent INR if on warfarin)
- Dental X-rays or records from a previous dentist, we can often incorporate existing imaging into our evaluation, though we may take a new CBCT for precise surgical planning
- Your dental insurance card, our team verifies your implant benefits before your appointment so you know your out-of-pocket cost upfront
- Your questions, write them down. The consultation is your opportunity to understand every aspect of the process, and no question is too basic
Patients from Sudbury, Framingham, Westborough, Southborough, and throughout MetroWest find that the evaluation process is thorough, educational, and entirely pressure-free. Many patients tell us it was the most informative dental appointment they have ever had.
Ready to assess your candidacy? Call (508) 481-0110 or book now.
Related Articles
- What to Expect During Dental Implant Surgery
- Do I Need a Bone Graft for a Dental Implant?
- The Real Cost of Dental Implants in Massachusetts
- Dental Implant Awareness Month: Benefits of Implants