Featured Answer: Why choose dental implants?
Dental implants are the only tooth replacement that preserves jawbone through osseointegration, prevents adjacent teeth from shifting, and restores full chewing force. A 2019 systematic review in the Clinical Oral Implants Research journal reported a 96.4% 10-year survival rate for modern implants, making them the most durable and predictable tooth replacement available. With proper care, a single implant can last 25 years or longer, often a lifetime.
Every September, Dental Implant Awareness Month highlights one of the most transformative advances in modern dentistry. For residents of Marlborough, MA and the greater MetroWest area, it's a good time to learn how implants restore both your smile and your daily quality of life. At Innova Smiles, Dr. Ambereen Fatima and our team use this month to educate the community about the life-changing benefits of implant dentistry, and to help patients understand why the upfront investment pays for itself many times over.
The Complete Benefits of Dental Implants
1. Bone Preservation and Facial Structure
This is the benefit that sets implants apart from every other tooth replacement. When a tooth is extracted or lost, the alveolar bone in that area begins to resorb (shrink) because it no longer receives stimulation from chewing forces transmitted through the tooth root. A study published in Clinical Oral Implants Research by Carlsson and Lindquist documented that the mandible (lower jaw) loses approximately 40% to 60% of its width within the first three years after tooth loss, with continued resorption averaging 0.5 to 1.0 mm per year thereafter.
This bone loss causes visible changes. The lower face collapses inward, the chin appears more pointed, lips lose support and thin out, and vertical facial height decreases. Patients who have worn full dentures for decades often have a distinctly sunken appearance that ages them well beyond their years.
Implants halt this process entirely. The titanium post integrates with the jawbone through osseointegration, the bone forms a direct structural and functional connection with the implant surface. Once integrated, the implant transmits chewing forces to the bone just as a natural root would, maintaining bone density and volume. The American Academy of Implant Dentistry (AAID) confirms that implants are the only restorative option that preserves and stimulates natural bone.
For patients in Westborough, Shrewsbury, and surrounding MetroWest communities who have been missing teeth for years, bone grafting procedures can rebuild lost bone and still make implant placement possible. Dr. Fatima evaluates bone density using 3D CBCT imaging at the initial consultation.
2. Adjacent Tooth Protection
A traditional dental bridge requires grinding down the two teeth on either side of the gap to serve as anchor supports. These healthy teeth lose 63% to 72% of their enamel during bridge preparation, according to data published in the Journal of Prosthetic Dentistry. Once a tooth is prepared for a bridge, it will always need a restoration.
An implant stands independently in the jawbone. It does not touch, lean on, or require modification of any neighboring teeth. The adjacent teeth remain completely intact, their enamel, structure, and long-term prognosis are unaffected.
Additionally, when a tooth is missing, the teeth on either side gradually drift into the empty space. This migration creates gaps, changes the bite relationship, and makes the area harder to clean, increasing the risk of decay and gum disease in adjacent teeth. An implant fills the space immediately and permanently, maintaining proper tooth alignment and spacing.
3. Full Restoration of Chewing Function
Missing teeth and ill-fitting dentures force dietary compromises that directly affect nutrition and overall health. A study in the Journal of Dental Research found that denture wearers chew with only 20% to 25% of the force of natural teeth. The National Institute of Dental and Craniofacial Research (NIDCR) reports that denture wearers frequently avoid fibrous vegetables, raw fruits, nuts, lean meats, and whole grains, precisely the foods that form the foundation of a heart-healthy diet.
Implants restore 85% to 100% of natural chewing force. Patients can bite into apples, eat corn on the cob, enjoy steak, and chew raw vegetables without worry about slippage, pain, or adhesive failure. For older adults in particular, this nutritional freedom has measurable health consequences. A 2018 study in Nutrients demonstrated that implant patients consumed significantly more fruits, vegetables, and fiber compared to denture wearers, with corresponding improvements in vitamin and mineral intake.
4. Speech Clarity
Loose or poorly fitting dentures can shift during speech, causing slurring, clicking, or a lisp, particularly with words containing "s," "f," and "th" sounds. Patients frequently report speaking more quietly or avoiding conversations because they are self-conscious about their dentures moving. Implants are fixed in the bone and do not shift. Speech clarity is fully restored from the day the final restoration is placed.
5. Elimination of Denture Adhesives
The daily routine of denture wearers includes applying adhesive paste, dealing with oozing at the margins, enduring an unpleasant taste, and spending time cleaning adhesive residue from both the denture and the palate each night. Implant-supported restorations, whether individual crowns, bridges, or full-arch prostheses, are permanently or semi-permanently attached. There is no adhesive, no daily removal for soaking, and no risk of the restoration dislodging during meals or conversation.
6. Psychological and Social Well-Being
The emotional impact of missing teeth is well documented and often underestimated. A 2023 study in the Journal of Prosthetic Dentistry found that patients who received dental implants reported statistically significant improvements in self-esteem (measured by the Rosenberg Self-Esteem Scale), social interaction confidence, and overall quality of life compared to patients using removable dentures. The Oral Health Impact Profile (OHIP-14) scores improved by an average of 58% in implant patients versus 23% in denture patients.
Patients describe stopping the habit of covering their mouth when they laugh, accepting dinner invitations they previously declined, smiling confidently in photographs, and feeling more comfortable in professional and social settings. These improvements are not secondary, for many patients, they are the primary reason they chose implants.
7. Convenience and Simplicity
Implants are cared for exactly like natural teeth. Brush twice daily, floss or use an interdental brush around the implant, and attend regular cleanings every six months. There is no special cleaning solution, no overnight soaking, no removal and reinsertion, and no dietary restrictions. The simplicity of maintenance is a significant quality-of-life advantage that patients consistently rank among the top benefits.
Who Benefits Most from Dental Implants?
- Adults missing one or more teeth who want a permanent, fixed solution that does not compromise adjacent teeth
- Denture wearers frustrated with slipping, adhesives, dietary limitations, and the daily maintenance routine
- Patients who have lost teeth due to injury, decay, or periodontal disease and want to prevent further bone loss
- Patients with failing bridges or large restorations that are reaching end of life
- Anyone seeking to prevent the bone resorption and facial changes that follow tooth loss
- Patients from Hudson, Framingham, Sudbury, and across MetroWest looking for experienced, fellowship-trained implant placement close to home
Implants vs. Bridges vs. Dentures: A 20-Year Cost Comparison
The upfront cost of implants is higher than alternatives, and that number understandably gives patients pause. But the long-term economics tell a different story.
| Factor | Single Implant | 3-Unit Bridge | Partial Denture |
|---|---|---|---|
| Initial cost | $3,000–$5,000 | $2,500–$4,500 | $700–$2,500 |
| Average lifespan | 25+ years (often lifetime) | 10–15 years | 5–8 years |
| Replacements in 20 years | 0 | 1–2 bridge replacements | 2–4 reline/remakes |
| 20-year total cost | $3,000–$5,000 | $5,000–$13,500 | $2,800–$10,000+ |
| Bone preservation | Yes | No | No (accelerates loss) |
| Adjacent tooth damage | None | Requires grinding 2 healthy teeth | Clasps can loosen teeth |
| Maintenance | Brush and floss normally | Floss threader required | Daily removal, soaking, adhesive |
A 2014 analysis in the Journal of Dental Research by Zeytinogl et al. concluded that single-tooth implants became the most cost-effective treatment option at the 14-year mark when compared to fixed partial dentures (bridges), accounting for replacement costs, complications, and maintenance. By year 20, implants cost approximately 40% less than the cumulative expense of bridge replacements.
Use our implant cost calculator to see what your specific investment might look like based on the number of teeth and your insurance coverage.
Implants vs. Dentures: More Than Just Cost
Traditional dentures rest on the gum ridge and rely on suction, adhesive, and the shape of the underlying bone for retention. As bone resorbs after tooth loss, the ridge flattens and denture fit deteriorates, a self-reinforcing cycle that worsens over time. The NIDCR notes that many long-term denture wearers eventually reach a point where no amount of adhesive can stabilize their prosthesis.
Implant-supported solutions break this cycle entirely. Options include:
- Individual implant crowns: One implant per missing tooth. Ideal for single-tooth gaps or scattered missing teeth.
- Implant-supported bridges: Two implants support a three-to-four-tooth bridge. No grinding of adjacent natural teeth required.
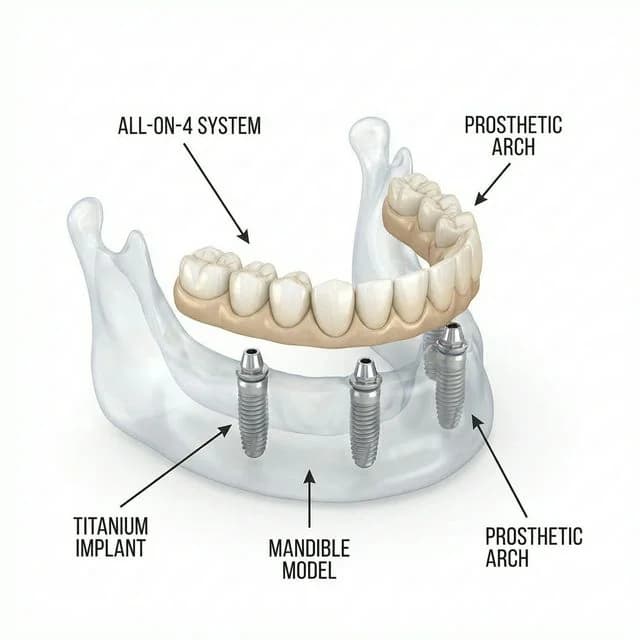
- Full-arch hybrid prostheses (All-on-4 / All-on-6): Four to six strategically placed implants support a full arch of fixed teeth. The entire upper or lower arch is restored in a single surgical session, often with a provisional prosthesis placed the same day. This approach is particularly transformative for patients currently wearing full dentures.
Advances in Implant Technology at Innova Smiles
Today’s implant procedures bear little resemblance to those of even a decade ago. At Innova Smiles, we use several technologies that improve precision, reduce surgical time, and enhance outcomes:
- 3D CBCT imaging: Cone Beam Computed Tomography produces a three-dimensional model of your jawbone, sinuses, nerves, and adjacent tooth roots. Dr. Fatima uses this to measure bone density at the exact implant site, determine the optimal implant size and angle, and identify anatomical structures that must be avoided, all before surgery begins.
- Guided surgical protocols: Using CBCT data, Dr. Fatima designs a custom surgical guide, a 3D-printed template that fits over your teeth and directs the drill to the precise planned position. Guided surgery reduces placement error to less than 1 mm, shortens surgical time, and minimizes tissue trauma. A 2018 meta-analysis in the International Journal of Oral and Maxillofacial Implants found that guided surgery reduced mean angular deviation by 78% compared to freehand placement.
- Digital impressions: The 3Shape TRIOS intraoral scanner captures a precise 3D model of your teeth and implant abutment without goopy impression material. Read more about this technology in our post on digital dental impressions.
- Advanced implant surfaces: Modern titanium implants feature micro-roughened and nano-textured surfaces that accelerate osseointegration. Where older implants required 6 to 9 months for full integration, current surface technology often achieves adequate stability in 3 to 4 months.
Dr. Fatima’s dual Fellowships — Fellow of the International Congress of Oral Implantologists (FICOI) and Fellow of the American Academy of Implant Prosthodontics (FAAIP), represent advanced surgical and prosthetic expertise that fewer than 5% of general dentists hold. These credentials reflect hundreds of hours of additional training in implant surgery, bone grafting, and implant prosthetics beyond dental school. To learn more about guided surgery, read our post on CBCT precision in implant placement.
The Implant Process: What to Expect Step by Step
Understanding the complete timeline removes much of the uncertainty that causes patients to delay treatment.
Phase 1: Consultation and Treatment Planning (Visit 1)
Dr. Fatima conducts a comprehensive examination including 3D CBCT scan, digital photographs, periodontal evaluation, and review of your medical history. This appointment determines:
- Whether you have sufficient bone for implant placement, or if bone grafting is needed first
- The optimal implant size, type, and angulation for your anatomy
- Whether any teeth need extraction before implant placement
- A complete treatment timeline and financial breakdown with insurance verification
Phase 2: Bone Grafting (If Needed — 3 to 6 Month Healing)
Patients who have been missing teeth for an extended period, or who had teeth extracted with significant bone loss, may need a bone graft before implant placement. Dr. Fatima uses allograft (processed donor bone) or xenograft (bovine-derived bone mineral) packed into the deficient area. The graft material serves as a scaffold for your own bone cells to regenerate new bone over 3 to 6 months. Not every patient requires grafting, many have adequate bone for immediate placement.
Phase 3: Implant Placement Surgery (Visit 2)
Using the surgical guide fabricated from CBCT data, Dr. Fatima places the titanium implant into the jawbone. The procedure is performed under local anesthesia, with gentle care options available for anxious patients. Key details:
- A single implant placement typically takes 30 to 60 minutes.
- Most patients report that the procedure was significantly more comfortable than they anticipated, comparable to having a filling placed.
- A healing cap is placed over the implant, and the surgical site is sutured.
- You leave with specific post-operative instructions, prescriptions if needed, and Dr. Fatima’s direct contact information.
Phase 4: Osseointegration (3 to 6 Months of Healing)
The implant integrates with the jawbone over this period. During healing, you can eat normally (avoiding the surgical site for the first week), work, exercise, and go about your life. If the implant is in a visible area, a temporary prosthesis maintains your appearance throughout this period.
Phase 5: Abutment and Final Crown (Visits 3–4)
Once osseointegration is confirmed (Dr. Fatima verifies stability with clinical testing and imaging), a small connector piece (abutment) is attached to the implant. A digital impression captures the exact shape and position. Your custom porcelain crown is fabricated by the lab and delivered at your final appointment. The crown is color-matched to your natural teeth and contoured to look and feel indistinguishable from the real thing.
The AAID notes that the total timeline from initial consultation to final crown ranges from 3 to 9 months, depending on whether bone grafting is needed. For detailed recovery information, see our post on implant recovery day by day.
Implant Success Rates and Longevity
Modern dental implants have among the highest success rates of any surgical procedure:
- Overall survival rate: 96.4% at 10 years (systematic review, Clinical Oral Implants Research, 2019)
- 20-year survival rate: 89.1% to 93.3% depending on jaw location (Lemos et al., Journal of Prosthodontic Research, 2016)
- Posterior mandible (lower back teeth): Highest success rates, typically exceeding 97%
- Maxillary (upper jaw): Slightly lower due to softer bone density; still above 93% at 10 years
Factors that improve long-term outcomes:
- Non-smoking status (smokers have 2 to 3 times higher failure rates)
- Well-controlled blood sugar in diabetic patients
- Adequate bone density at the implant site
- Regular professional maintenance every 6 months
- Good daily oral hygiene around the implant
- Wearing a night guard if you clench or grind (bruxism generates forces that can stress implant components)
Implant Care After Placement
Caring for implants is straightforward and very similar to caring for natural teeth:
- Brush twice daily with a soft-bristled toothbrush, angling the bristles toward the gumline around the implant
- Clean between the implant and adjacent teeth using an interdental brush (TePe or GUM brand), a water flosser (Waterpik), or implant-specific floss. Traditional floss works but can shred against the abutment; unwaxed tape floss or a floss threader provides better results.
- Professional cleanings every six months. Our hygienists use plastic or titanium-tipped scalers specifically designed for implant surfaces, standard metal instruments can scratch the titanium.
- Avoid tobacco. Smoking increases peri-implantitis (inflammation around the implant) risk by 3 to 4 times.
- Maintain stable blood sugar if you are diabetic. Uncontrolled diabetes impairs healing and increases the risk of implant failure.
- Wear a night guard if you clench or grind. Excessive lateral forces can fracture the porcelain crown or loosen the abutment screw.
Common Misconceptions About Dental Implants
"I’m too old for implants." Age alone is not a contraindication. Research published in Gerodontology found that implant success rates in patients over 80 were comparable to those in younger adults. General health, bone availability, and healing capacity matter far more than chronological age. Patients in their 70s and 80s routinely receive implants at Innova Smiles with excellent outcomes.
"Implant surgery is extremely painful." Most patients report that the surgery itself, performed under local anesthesia, is less uncomfortable than a tooth extraction. Post-operative discomfort is typically managed with ibuprofen for two to three days. A 2015 patient experience study in the International Journal of Oral and Maxillofacial Surgery found that 91% of implant patients rated their pain as "less than expected."
"My body will reject the implant." Titanium is biocompatible, it does not trigger an immune rejection response. Implant "failure" is almost always caused by infection (peri-implantitis), insufficient bone integration due to smoking or uncontrolled diabetes, or biomechanical overload, not immunological rejection.
"Implants are only for single missing teeth." Implants support everything from single crowns to full-arch fixed prostheses. From a single missing tooth to a full upper or lower arch, there is an implant solution designed for your situation.
Schedule Your Implant Consultation
Patients from Marlborough, Northborough, Southborough, Framingham, Hudson, and across MetroWest trust Dr. Fatima for implant placement because of her dual fellowship training, 3D-guided surgical precision, and commitment to conservative treatment planning. Every implant case at Innova Smiles starts with a thorough consultation, there is no pressure, just information and a clear treatment plan.
Ready to learn if implants are right for you? Call (508) 481-0110 or book online.
Related Articles
- Am I a Candidate for Dental Implants?
- Dental Implant vs. Bridge: Best Solution for Missing Teeth
- The Real Cost of Dental Implants in Massachusetts