Featured Answer: Why Do My Gums Bleed When I Brush My Teeth?
The most common reason gums bleed during brushing is gingivitis, the earliest stage of gum disease. Plaque (a sticky film of bacteria) accumulates along the gumline, and the body's immune system responds with inflammation. That inflammation makes the gum tissue fragile, swollen, and prone to bleeding on contact. The CDC reports that 47.2% of American adults over 30 have some form of periodontal disease, and many cases begin with this exact symptom: pink in the sink after brushing. The good news is that gingivitis is fully reversible. A professional cleaning and consistent home care can restore gum health completely, but only if you act on the warning sign rather than ignoring it. At Innova Smiles in Marlborough, Dr. Fatima evaluates gum health at every visit, measuring pocket depths and checking for bleeding on probing to catch disease at its earliest, most treatable stage.
"My Gums Always Bleed — That Is Just Normal for Me"
This is one of the most dangerous misconceptions in dentistry. Healthy gums do not bleed. Period. If the skin on your hand bled every time you washed it, you would see a doctor immediately. Gum tissue deserves the same response.
The normalization of bleeding gums is widespread. In a 2015 survey by the American Academy of Periodontology (AAP), more than one-third of Americans (36%) said they would rather do an unpleasant activity like cleaning the toilet (14%), washing a sink full of dishes (18%), or waiting in a long checkout line (14%) than floss their teeth, and many cited bleeding as the reason they avoid flossing altogether. The irony is that stopping flossing because of bleeding makes the problem worse, not better. The bleeding is a signal that bacteria are winning the battle at the gumline, and the solution is more cleaning, not less.
Understanding why gums bleed, and what to do about it, can prevent you from joining the nearly 65 million American adults the CDC estimates have moderate to severe periodontitis.
The Most Common Cause: Gingivitis
Gingivitis accounts for the vast majority of bleeding gum cases. Here is how the process works:
The Plaque-to-Bleeding Pipeline
-
Plaque forms. Within hours of brushing, a new layer of bacterial plaque begins forming on tooth surfaces. This is normal and unavoidable, it happens to everyone.
-
Plaque accumulates at the gumline. If plaque is not removed through brushing and flossing within 24 to 48 hours, it thickens and begins irritating the gum tissue where it contacts the tooth.
-
The immune system responds. Your body sends white blood cells and inflammatory mediators to the area to fight the bacteria. This response causes the classic signs of inflammation: redness, swelling, and warmth.
-
Blood vessels dilate and become fragile. Increased blood flow to the inflamed area engorges the tiny capillaries in the gum tissue. These dilated vessels are close to the surface and break easily with even light pressure, the pressure of a toothbrush bristle or a strand of floss.
-
You see blood. Pink on your toothbrush, red-tinged spit in the sink, or blood on your floss.
-
If untreated, plaque hardens into tartar (calculus). Within 48 to 72 hours, minerals in saliva begin to calcify plaque into tartar, a hard deposit that cannot be removed with a toothbrush. Tartar provides a rough surface that attracts more plaque, accelerating the cycle. Only professional instruments (ultrasonic scalers and hand curettes) can remove tartar.
Patients from Hudson and Framingham often arrive at Innova Smiles saying they have "sensitive gums" when what they actually have is gingivitis. The distinction matters because sensitivity suggests a permanent condition you have to live with, while gingivitis is a treatable, reversible disease.
Other Causes of Bleeding Gums
While gingivitis is the most common explanation, several other conditions can cause gums to bleed:
Brushing Too Hard or Using Hard Bristles
Aggressive brushing with a hard-bristled brush can physically traumatize gum tissue, causing it to bleed even when no disease is present. The ADA recommends a soft-bristled brush for all patients. You should brush with gentle pressure, think of it as massaging the gums, not scrubbing them. If your bristles are splayed flat after a few weeks, you are pressing too hard.
Electric toothbrushes with pressure sensors (like the Oral-B iO or Sonicare DiamondClean) can help. They alert you, with a light, vibration, or sound, when you are applying too much force.
Starting a New Flossing Routine
If you have not flossed regularly and then begin, your gums will likely bleed for the first few days to two weeks. This is because the tissue is already inflamed from bacterial buildup between teeth. The bleeding is not a reason to stop, it is confirmation that those areas needed attention. In most cases, daily flossing reduces and eliminates the bleeding within 10 to 14 days as inflammation subsides.
If bleeding from flossing persists beyond two weeks despite consistent daily use, the inflammation may be more advanced than simple gingivitis, and a professional evaluation is warranted.
Medications: Blood Thinners and Anticoagulants
Several categories of medication increase bleeding tendency, including from the gums:
| Medication | Type | Common Brand Names |
|---|---|---|
| Warfarin | Anticoagulant | Coumadin, Jantoven |
| Aspirin | Antiplatelet | Bayer, Ecotrin |
| Clopidogrel | Antiplatelet | Plavix |
| Apixaban | DOAC (Direct Oral Anticoagulant) | Eliquis |
| Rivaroxaban | DOAC | Xarelto |
| Dabigatran | DOAC | Pradaxa |
If you take any of these medications and notice increased gum bleeding, tell both your prescribing physician and your dentist. Do not stop taking blood thinners without medical advice, the risk of stroke or blood clot is far more serious than gum bleeding. Instead, work with your dental team to manage gum health more aggressively to minimize inflammation and the bleeding it causes.
Pregnancy Gingivitis
Hormonal changes during pregnancy, particularly elevated progesterone levels, increase blood flow to the gums and amplify the inflammatory response to plaque. The result is a condition called pregnancy gingivitis, which affects 60 to 75% of pregnant women according to the American Pregnancy Association.
Symptoms typically appear in the second trimester and peak in the third. Gums become puffy, red, and bleed easily during brushing and flossing. In some cases, a localized swelling called a pregnancy granuloma (or pyogenic granuloma) develops on the gumline, a round, red growth that bleeds readily. These are benign and usually resolve after delivery, but may need removal if they interfere with eating or oral hygiene.
For expecting mothers in Southborough and Northborough, Dr. Fatima recommends scheduling a dental cleaning during the second trimester and maintaining diligent home care throughout pregnancy. Professional cleanings during pregnancy are safe and recommended by both the ADA and the American College of Obstetricians and Gynecologists (ACOG).
Vitamin Deficiencies
Vitamin C deficiency (scurvy). While severe scurvy is rare in the United States, marginal vitamin C deficiency is more common than many people realize, especially in older adults, smokers, and people with restrictive diets. Vitamin C is necessary for collagen synthesis, and without adequate collagen, gum tissue becomes fragile and bleeds easily. A 2021 study in Nutrition Reviews found that plasma vitamin C levels were inversely associated with periodontal disease severity. Daily intake of vitamin C-rich foods (citrus fruits, bell peppers, broccoli, strawberries, kiwi) supports gum tissue integrity.
Vitamin K deficiency. Vitamin K is necessary for blood clotting. Deficiency, which can result from malabsorption syndromes, prolonged antibiotic use, or liver disease, increases bleeding tendency throughout the body, including the gums. Green leafy vegetables (kale, spinach, broccoli) are the primary dietary source of vitamin K.
Poorly Fitting Dentures or Dental Appliances
Dentures, retainers, or orthodontic appliances that do not fit properly can irritate gum tissue and cause localized bleeding. If you wear a removable appliance and notice bleeding in a specific area, have the fit checked by your dentist.
Systemic Conditions
In some cases, bleeding gums are a sign of a systemic medical condition rather than a local dental problem:
- Diabetes. Uncontrolled diabetes impairs immune function and increases susceptibility to periodontal infections. The relationship is bidirectional, gum disease makes blood sugar harder to control, and high blood sugar makes gum disease worse. The American Diabetes Association recommends that all diabetic patients receive periodontal evaluation and treatment as part of their diabetes management plan.
- Leukemia. Bleeding, swollen gums can be an early sign of leukemia, particularly acute leukemia. The abnormal white blood cells infiltrate gum tissue, causing enlargement and spontaneous bleeding. While this is an uncommon cause, it is an important one, especially when bleeding is accompanied by fatigue, easy bruising, or frequent infections.
- Thrombocytopenia. Low platelet count from any cause (medications, autoimmune conditions, bone marrow disorders) reduces the body's ability to form clots, leading to prolonged bleeding from minor gum trauma.
- Liver disease. The liver produces clotting factors. Advanced liver disease impairs clotting factor production, increasing bleeding risk.
Should I Keep Brushing if My Gums Bleed?
Yes — without question.
This is the question patients ask most often, and the answer surprises many of them. Stopping brushing because your gums bleed is like stopping hand-washing because your infected cut stings. The discomfort is a sign that the area needs more attention, not less.
Here is what happens when you keep brushing despite bleeding:
- Days 1–3: Bleeding may initially seem the same or slightly worse as you are now disrupting bacterial colonies that have been undisturbed.
- Days 4–7: Bleeding begins to decrease. The bacterial load is dropping, and the inflammatory response is starting to subside.
- Days 7–14: Most areas that were bleeding will have stopped. Gum tissue is getting firmer and pinker.
- Days 14–21: Gums should look and feel healthier. Bleeding may persist only in areas with tartar buildup that requires professional removal.
The key is technique. Use a soft-bristled brush. Angle the bristles 45 degrees toward the gumline. Use gentle, short strokes, not aggressive scrubbing. Let the bristles do the work. And floss daily, even if the floss comes out bloody at first.
If bleeding persists beyond three weeks of consistent, proper brushing and flossing, you likely have tartar deposits that need professional removal. Schedule a cleaning.
When Bleeding Gums Signal Serious Gum Disease
While occasional, minor bleeding during brushing is commonly a sign of early gingivitis, certain patterns of bleeding indicate more advanced periodontal disease that needs prompt treatment:
Spontaneous bleeding. Gums that bleed without any provocation, blood on your pillow, blood in your saliva during the day, suggest significant inflammation and possible advanced periodontitis.
Bleeding accompanied by loose teeth. If you notice a tooth shifting position, feeling mobile, or biting differently, the bone supporting that tooth has likely been compromised by periodontal disease.
Bleeding with pus (suppuration). A foul taste or visible pus along the gumline indicates an active periodontal abscess, a bacterial infection that requires professional drainage and treatment.
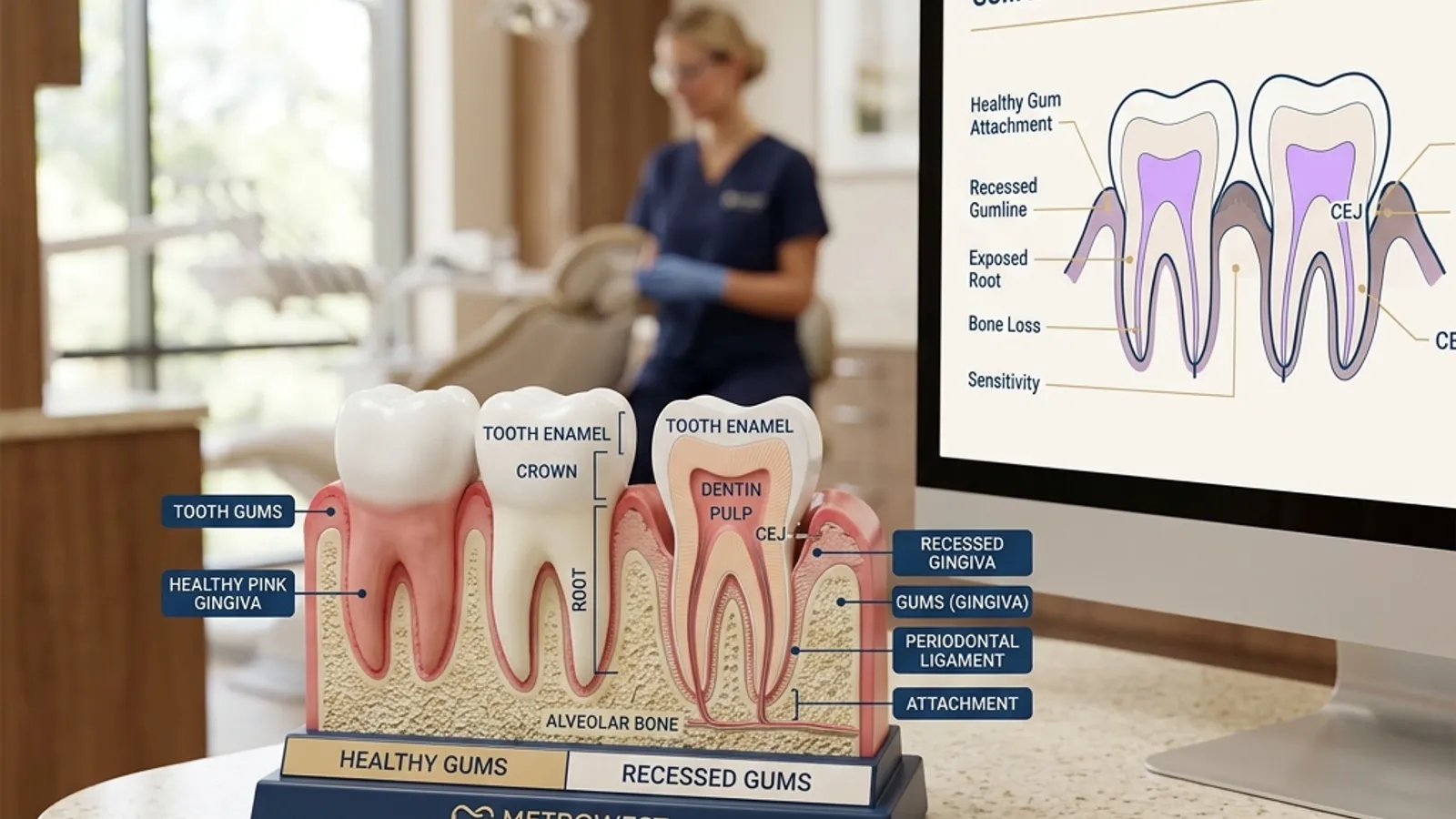
Bleeding with receding gums. If your teeth look longer than they used to, or if you can see yellow root surfaces that were previously covered, gum recession from periodontal disease is exposing vulnerable tooth structure.
Bleeding with persistent bad breath. Chronic halitosis that does not improve with brushing, flossing, and tongue cleaning often indicates deeper periodontal pockets harboring anaerobic bacteria. These bacteria produce volatile sulfur compounds with a characteristic sulfur/rotten egg smell.
If you are experiencing any combination of these symptoms, schedule an evaluation rather than waiting for your next routine cleaning. Patients from Westborough and Shrewsbury can call Innova Smiles for a focused periodontal assessment.
What Happens at a Dental Visit for Bleeding Gums
When you come to Innova Smiles with bleeding gum concerns, here is what the evaluation looks like:
Periodontal Probing
Your hygienist uses a thin, calibrated instrument called a periodontal probe to measure the depth of the space (sulcus or pocket) between each tooth and the surrounding gum tissue. Six measurements are taken per tooth, three on the cheek side, three on the tongue side. Healthy sulcus depth is 1 to 3 millimeters. Depths of 4 millimeters or greater indicate periodontal pocketing and likely bone loss.
Bleeding on Probing (BOP) Score
As the probe gently touches the gum tissue at the base of each sulcus, the hygienist records whether bleeding occurs. The percentage of sites that bleed, the BOP score, is one of the most reliable indicators of active gum inflammation. A BOP score above 10% indicates clinically significant inflammation. In active periodontitis, BOP scores can exceed 50%.
Digital X-Rays
Periapical and bitewing radiographs reveal bone levels around each tooth. In healthy mouths, bone reaches within 1 to 2 millimeters of the junction where the crown meets the root. In periodontal disease, the bone level drops, creating characteristic patterns of horizontal or vertical bone loss. Comparing current X-rays to previous films shows whether bone loss is stable or progressing.
Clinical Assessment
Dr. Fatima evaluates tooth mobility (using a scale of 0 to 3), checks for furcation involvement (bone loss between the roots of multi-rooted teeth), assesses gum recession, and examines for signs of occlusal trauma (excessive biting forces that can accelerate periodontal breakdown).
The Treatment Ladder: From Simple to Advanced
Treatment depends on the severity of disease:
Level 1: Improved Home Care (Gingivitis Without Tartar Buildup)
If probing depths are normal (1 to 3 millimeters) and the bleeding is caused by inadequate brushing or flossing technique, the treatment is education and coaching. Your hygienist will demonstrate proper brushing angle, flossing technique, and may recommend specific tools (interdental brushes, a water flosser, or an electric toothbrush).
Level 2: Professional Cleaning / Prophylaxis (Gingivitis With Tartar)
When tartar (calculus) is present above or just below the gumline, a standard prophylaxis removes it and allows the gum tissue to heal. This is what most people know as a "regular cleaning." For patients with gingivitis, a single cleaning combined with improved home care resolves the condition in 2 to 4 weeks.
Level 3: Scaling and Root Planing / SRP (Early to Moderate Periodontitis)
When pockets reach 4 to 6 millimeters and bone loss is present on X-rays, scaling and root planing, commonly called a "deep cleaning", is the standard treatment. SRP uses ultrasonic and hand instruments to remove bacterial deposits and tartar from deep within periodontal pockets, below the gumline. The root surfaces are smoothed (planed) to discourage bacterial reattachment. Treatment is performed under local anesthesia, usually over two appointments (one per side).
Patients from Hopkinton and Sudbury who need SRP often ask whether it hurts. With proper anesthesia, the procedure itself is comfortable. Some tenderness for 24 to 48 hours afterward is normal and resolves with over-the-counter pain relievers.
Level 4: Periodontal Maintenance (Post-SRP Ongoing Care)
After scaling and root planing, patients transition from standard 6-month cleanings to periodontal maintenance every 3 to 4 months. These more frequent visits allow the hygienist to monitor pocket depths, remove bacterial regrowth before it causes further damage, and catch any signs of disease progression early. Periodontal maintenance is not just a "more frequent cleaning", it is a targeted, therapeutic procedure that focuses on previously diseased sites.
Level 5: Surgical Intervention (Advanced Periodontitis)
When pockets exceed 6 millimeters and SRP alone cannot adequately access and clean the root surfaces, surgical intervention may be recommended. Options include flap surgery (reflecting gum tissue to access and clean deep pockets), bone grafting (to regenerate lost bone), and guided tissue regeneration (using membranes to direct bone growth into defects). These procedures are typically performed by a periodontist.
How to Stop Your Gums From Bleeding at Home
For patients with early gingivitis (bleeding but no bone loss), these steps can resolve the problem within two to four weeks:
Use a soft-bristled toothbrush. Hard and medium bristles traumatize gum tissue. The ADA recommends soft bristles for everyone.
Brush for two full minutes, twice daily. Most people brush for 45 to 60 seconds, which is not long enough to adequately clean all surfaces. An electric toothbrush with a built-in timer ensures you reach the full two minutes.
Angle your brush at 45 degrees toward the gumline. This targets the critical area where plaque accumulates, the sulcus between the tooth and gum. Short, gentle back-and-forth strokes or circular motions are most effective.
Floss daily. Flossing removes plaque and food debris from between teeth where your toothbrush cannot reach. Wrap the floss into a C-shape around each tooth and slide it gently below the gumline. If traditional floss is difficult, interdental brushes (like TePe or GUM Proxabrush) or a water flosser (Waterpik) are effective alternatives.
Use an antiseptic mouthwash. Rinses containing cetylpyridinium chloride (CPC) or chlorhexidine reduce bacterial counts in the mouth. Chlorhexidine (Peridex) is prescription-strength and the most effective, but it can stain teeth with prolonged use and is typically used short-term. CPC-based rinses (Crest Pro-Health, Colgate Total) are available over the counter for daily use.
Stay hydrated. Adequate water intake supports saliva production, which is your mouth's primary defense against bacterial buildup.
When to See a Dentist Urgently vs. Waiting for Your Next Cleaning
See your dentist soon (within a few days) if you experience:
- Bleeding that does not improve after 2 to 3 weeks of consistent brushing and flossing
- Bleeding accompanied by swelling, pain, or a bad taste
- A single area that bleeds much more than others
- Bleeding gums plus tooth sensitivity or mobility
See your dentist promptly (within 24 to 48 hours) if you experience:
- Spontaneous bleeding from the gums without brushing or flossing
- Pus or discharge from the gumline
- Sudden looseness of one or more teeth
- Severe gum swelling that affects eating or swallowing
The Gum Disease–Systemic Health Connection
Bleeding gums are not just a dental problem. Decades of research have established associations between periodontal disease and several serious systemic conditions:
Cardiovascular disease. A 2020 consensus report from the European Federation of Periodontology (EFP) and the World Heart Federation confirmed a consistent epidemiological association between periodontitis and atherosclerotic cardiovascular disease. Periodontal bacteria have been found in atherosclerotic plaques, and chronic periodontal inflammation is believed to contribute to systemic vascular inflammation.
Diabetes. The relationship between diabetes and gum disease is bidirectional and well-established. A 2018 joint report from the AAP and the European Federation of Periodontology stated that treating periodontal disease can reduce HbA1c levels by 0.27 to 0.48 percentage points, a clinically meaningful improvement in blood sugar control.
Adverse pregnancy outcomes. Multiple studies have linked untreated periodontitis to increased risk of preterm birth and low birth weight. While the evidence is still evolving, the potential risk reinforces the importance of gum health during pregnancy.
Respiratory infections. Aspiration of oral bacteria into the lungs can contribute to pneumonia, particularly in elderly or immunocompromised patients. Maintaining oral hygiene reduces this risk.
For a deeper look at these connections, see our articles on the oral health–heart disease connection and dental care and diabetes.
Schedule a Gum Health Evaluation
If you see blood when you brush, do not wait and hope it resolves on its own. In most cases, the treatment is straightforward, a professional cleaning and some home care adjustments, but the longer you wait, the more the disease progresses and the more involved treatment becomes.
Innova Smiles is located at 340 Maple St, Suite 100, Marlborough, MA 01752, serving patients from Natick, Framingham, Westborough, Hudson, and communities throughout MetroWest Massachusetts. Call (508) 481-0110 or book your appointment online.
Concerned about bleeding gums? Call (508) 481-0110 or schedule a gum health evaluation.
Related Articles
- The 4 Stages of Gum Disease: Early Signs, Risks, and Treatment
- Gum Recession: Causes, Signs, and Treatment
- Deep Cleaning vs. Regular Cleaning: Understanding SRP
- The Connection Between Oral Health and Heart Disease