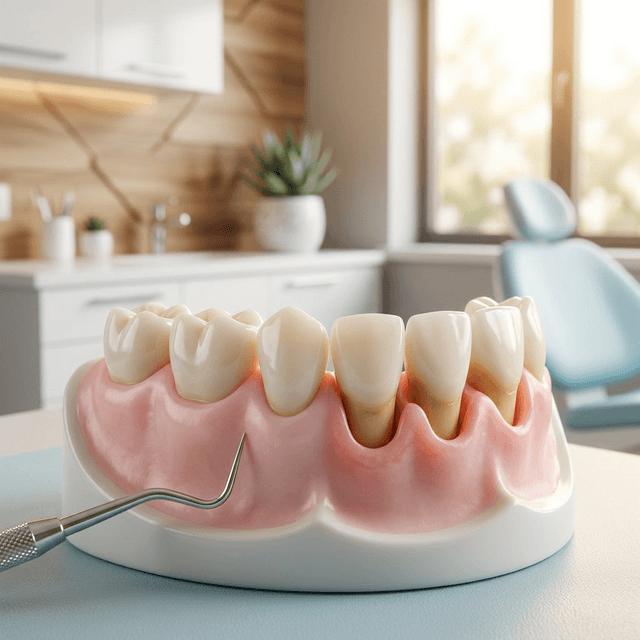
Gum recession is one of the most underdiagnosed dental problems--because it usually happens slowly, over years, without causing obvious pain. By the time most patients notice it, significant tissue loss has already occurred. If left untreated, gum recession leads to root sensitivity, increased cavity risk, and eventually tooth loss. At Innova Smiles in Marlborough, we see patients from Hudson, Sudbury, and surrounding MetroWest towns who are concerned about receding gums and want to understand their treatment options.
The good news: caught early, gum recession is manageable. Here is a thorough clinical guide.
What Is Gum Recession?
Gum recession occurs when the marginal gingival tissue that surrounds teeth migrates apically (toward the root), exposing the root surface that is normally protected beneath the gumline. You might notice:
- Teeth that look "longer" than they used to
- A visible notch or step where the gum meets the tooth
- Increased sensitivity, especially to cold, sweet, or acidic foods
- Roots that feel rougher than the crown portion of the tooth
- Yellow or darker coloring near the gumline where root dentin is exposed
Unlike tooth enamel (the hardest substance in the human body, rated 5 on the Mohs scale), the exposed root surface is covered only by cementum--a much softer mineral layer only 20 to 50 micrometers thick. Once that thin cementum wears away, the underlying root dentin is directly exposed to bacteria, temperature changes, and mechanical abrasion. Root surfaces decay at a pH of 6.7, compared to 5.5 for enamel, which means root cavities develop faster and in less acidic conditions.
How Common Is Gum Recession?
Extremely common. Research published in the Journal of Periodontology (Kassab & Cohen, 2003) found that approximately 50% of people aged 18 to 64 have at least one site of measurable gum recession. The National Institute of Dental and Craniofacial Research (NIDCR) confirms that recession prevalence rises with age--by age 65, nearly 88% of adults have at least one tooth with recession of 1mm or more. Many of these patients are unaware because the process is gradual and often asymptomatic until it reaches an advanced stage.
A 2015 study in the Journal of Clinical Periodontology (Jati et al.) further categorized recession by severity: Miller Class I and II defects (where bone and papilla between teeth remain intact) carry an excellent prognosis with grafting, while Miller Class III and IV defects (where bone loss has occurred between teeth) have progressively less predictable outcomes. This classification matters because it directly determines which treatment options will work for you.
What Causes Gum Recession?
Multiple factors contribute, and most patients have more than one working against them simultaneously:
1. Periodontal (Gum) Disease
The most common cause of generalized recession. Bacterial biofilm and calculus below the gumline trigger a chronic inflammatory response that destroys both gum tissue and the underlying alveolar bone. As bone height decreases, the gum tissue follows it apically. The Journal of Periodontology reports that patients with untreated periodontitis lose an average of 0.5 to 1.0mm of attachment per year. Untreated, this progresses to tooth mobility and eventual loss.
2. Aggressive Brushing (Toothbrush Abrasion)
Brushing with a hard-bristled toothbrush or applying excessive lateral pressure wears away gum tissue mechanically over time. This type of recession typically appears on the facial (cheek-side) surfaces of teeth--particularly canines and premolars that sit at the "corner" of the arch and receive the most brushing force. Many patients are surprised to learn that "brushing harder" causes more harm than good. A study in the Journal of Clinical Periodontology (DK Hooper et al., 2018) found that brushing force above 200 grams significantly increased recession risk. Most powered toothbrushes now include pressure sensors for this reason.
3. Thin Tissue Biotype (Genetics)
Some people inherit thinner gum tissue (called a thin or scalloped biotype) that is inherently more prone to recession regardless of oral hygiene habits. If you can see the outline of tooth roots through your gum tissue when you pull your lip back, you likely have a thin biotype. Roughly 30% of the population falls into this category.
4. Teeth Grinding and Clenching (Bruxism)
Chronic parafunctional forces of 300 to 800 pounds per square inch strain the periodontal ligament and supporting tissues, causing what periodontists call "occlusal trauma." This doesn't directly destroy gum tissue, but it accelerates recession in areas already weakened by inflammation or thin tissue. We fabricate custom night guards at Innova Smiles specifically to reduce this destructive load.
5. Misaligned Bite or Crooked Teeth
When individual teeth are crowded, rotated, or positioned labially (pushed outward from the arch), the bone and gum tissue over those teeth is thinner and more vulnerable to recession. This is especially common on lower front teeth that have shifted over time. Orthodontic treatment with Invisalign clear aligners or Spark aligners can reposition teeth into thicker bone, which often stabilizes recession.
6. Lip or Tongue Piercings
Jewelry that chronically rubs against gum tissue causes localized mechanical trauma. A study in The Journal of the American Dental Association found that 35% of patients with lip piercings had measurable recession on adjacent teeth within two years.
7. Tobacco Use
Smoking constricts blood vessels in gum tissue, reducing the delivery of oxygen and immune cells needed for tissue maintenance and repair. Smokers have 2 to 3 times the recession risk of non-smokers and respond less predictably to grafting procedures. Smokeless (chewing) tobacco causes direct chemical and mechanical damage to the tissue it contacts.
8. Frenum Attachment
A high or thick frenum (the small fold of tissue connecting the lip or cheek to the gum) can exert pulling force on the gingival margin, contributing to localized recession. This is particularly common on lower central incisors and upper lateral incisors. A frenectomy (simple tissue release) can eliminate this tension.
Warning Signs to Watch For
- Sensitivity: Sudden sensitivity to cold drinks, cold air, or sweet foods specifically at the gumline
- Visible elongation: Teeth appear noticeably longer compared to old photos
- Gumline notching: A visible step or indentation where the gum meets the tooth, sometimes with a wedge-shaped abrasion
- Root exposure: Darker-colored or yellow root surface visible below the enamel line
- Loose teeth: Advanced gum disease combined with bone loss
- Food impaction: Food gets stuck at the gumline more than it used to
- Bleeding when flossing: A sign of active inflammation that may be driving recession
Measuring Recession: The Miller Classification
Periodontists classify gum recession into four categories that determine treatment options and prognosis:
| Miller Class | Description | Grafting Prognosis |
|---|---|---|
| Class I | Recession does not extend beyond the mucogingival junction; no bone or tissue loss between teeth | Complete root coverage expected (95%+) |
| Class II | Recession extends beyond the mucogingival junction; no bone or tissue loss between teeth | Complete root coverage expected (90%+) |
| Class III | Bone or tissue loss between teeth is present, or tooth is malpositioned | Partial root coverage achievable |
| Class IV | Severe bone loss between teeth | Root coverage not predictable; focus on stabilization |
Dr. Fatima measures recession depth at every hygiene appointment using a periodontal probe--a comfortable measurement that takes about 30 seconds per tooth. Tracking these numbers over time reveals whether recession is stable or progressing, which directly guides treatment decisions.
Gum Recession Treatment Options
Treatment depends on severity, cause, and how many sites are affected. Mild recession can be managed conservatively; moderate to severe recession may require surgical correction.
For Mild Recession: Conservative Management
- Scaling and root planing (deep cleaning): Removes bacterial biofilm and calculus from below the gumline, eliminating the inflammatory trigger. Inflamed tissue can heal and partially reattach to the root surface. For more on this procedure, see our guide to deep cleaning vs. regular cleaning.
- Technique correction: Switching to a soft-bristled brush (manual or powered) and using the modified Bass technique--angling bristles 45 degrees toward the gumline with gentle circular strokes--stops mechanical recession in its tracks.
- Night guard therapy: A custom occlusal splint distributes grinding forces across all teeth, reducing the concentrated stress that accelerates recession on vulnerable teeth.
- Desensitizing treatments: Professional fluoride varnish (5% sodium fluoride), potassium nitrate toothpaste (such as Sensodyne), or resin bonding agents applied to exposed root surfaces block the open dentinal tubules that transmit pain signals. Relief is often immediate with professional application.
- Chlorhexidine rinse: For patients with active periodontal disease driving recession, a two-week course of 0.12% chlorhexidine gluconate reduces bacterial load while tissue heals.
For Moderate to Severe Recession: Surgical Options
- Connective tissue graft (CTG): The gold standard. According to the American Academy of Periodontology (AAP), a small strip of connective tissue is harvested from beneath the palatal mucosa (roof of mouth) and sutured over the exposed root. The graft integrates with existing tissue, providing a thicker, more resilient gum margin. A 2014 Cochrane review found that CTG achieves complete root coverage in 60 to 80% of cases and partial coverage in over 95% of Miller Class I and II defects. Healing takes two to three weeks, and most patients manage discomfort with ibuprofen alone.
- Free gingival graft (FGG): A thicker tissue graft taken from the surface of the palate, used primarily to increase the width of attached gingiva rather than to achieve root coverage. This is commonly used on lower front teeth where tissue is very thin.
- Pinhole surgical technique (PST): A newer, minimally invasive approach developed by Dr. John Chao. A small entry point is made in existing gum tissue with a needle, and the tissue is gently loosened and repositioned coronally (upward) over the exposed roots. Collagen strips are placed through the pinhole to stabilize the tissue in its new position. Recovery is faster than traditional grafting, with minimal swelling and no palatal donor site.
- Guided tissue regeneration (GTR): When bone loss accompanies recession, a resorbable membrane is placed over the defect to exclude fast-growing epithelial cells, allowing slower-growing bone and periodontal ligament cells to regenerate the lost attachment. This is often combined with bone graft material.
- Acellular dermal matrix (AlloDerm): A processed human tissue graft that eliminates the need for a palatal donor site. Clinical outcomes are comparable to CTG in many studies, and patients experience less post-operative discomfort because there is no palatal wound.
At Innova Smiles, we perform conservative recession management and coordinate with trusted periodontists in the MetroWest area when surgical intervention is indicated. Dr. Fatima ensures seamless communication between your restorative and periodontal care.
Gum Grafting Cost: What to Expect
Gum grafting costs in the Marlborough, MA area depend on the technique, number of teeth treated, and whether a tissue bank graft is used instead of a palatal harvest:
| Procedure | Typical Cost Per Site |
|---|---|
| Connective tissue graft (CTG) | $600–$1,200 |
| Free gingival graft (FGG) | $500–$1,000 |
| Pinhole surgical technique | $800–$1,500 |
| AlloDerm (acellular dermal matrix) | $700–$1,300 |
Many PPO dental insurance plans cover a portion of gum grafting when recession is documented and treatment is deemed medically necessary--typically under periodontal surgical benefits. We submit pre-authorization before scheduling so you know your out-of-pocket cost upfront. We also offer 0% financing through CareCredit and Cherry for patients who prefer monthly payments.
What Happens If Gum Recession Is Left Untreated?
Ignoring recession creates a cascade of increasingly serious problems:
- Root cavities: Exposed cementum and dentin decay much faster than enamel. A study in Caries Research found that root surface caries progress 2.5 times faster than coronal caries. Root cavities are also harder to restore because of their location and moisture control challenges.
- Worsening recession: Once tissue has receded, the thinner remaining margin is more vulnerable to further loss. The cycle accelerates without intervention.
- Chronic tooth sensitivity: What starts as occasional twinges from cold drinks becomes daily pain that affects eating, breathing in cold MetroWest winter air, and quality of life.
- Bone loss: Gum disease causing recession simultaneously destroys the alveolar bone that holds teeth in place. By the time teeth feel loose, significant bone has already been lost.
- Esthetic concerns: Dark triangles between teeth (black triangles) and uneven gumlines become more pronounced as recession progresses.
- Tooth loss: In advanced cases, teeth become mobile and eventually require extraction--followed by costly replacement with implant-supported options or bridges.
The cost of ignoring recession--in terms of both treatment complexity and expense--far exceeds the cost of early intervention. A $600 gum graft today can prevent a $5,000 implant five years from now.
Preventing Gum Recession
Prevention is straightforward once you understand the risk factors:
- Use a soft-bristled toothbrush--the ADA recommends soft bristles for everyone, and electric toothbrushes with pressure sensors (such as Oral-B iO or Sonicare) add an extra layer of protection
- Brush gently using the modified Bass technique: angle bristles 45 degrees toward the gumline, use small circular motions, and let the bristles do the work--not arm pressure
- Floss daily--it is the only way to remove bacterial plaque from between teeth and below the gumline where your toothbrush cannot reach
- See your dentist every 6 months for professional cleaning and recession measurement. Patients with a history of recession or periodontal disease benefit from every-3-to-4-month maintenance intervals.
- Wear a custom night guard if you grind your teeth--over-the-counter guards from pharmacies do not fit precisely and can actually worsen jaw problems
- Quit tobacco--or never start. Smoking cessation programs through your primary care provider can help, and your gum tissue begins to recover blood flow within weeks of quitting
- Address orthodontic issues that place teeth in vulnerable positions--aligner treatment can move teeth into thicker bone and improve long-term tissue stability
The Link Between Gum Recession and Overall Health
Periodontal disease--the most common driver of recession--is linked to systemic conditions that affect many MetroWest residents. Research published in the American Heart Association's Circulation journal has established associations between chronic periodontal infection and increased cardiovascular risk. Patients with uncontrolled type 2 diabetes are three times more likely to develop severe periodontal disease, which in turn makes blood sugar harder to control, creating a destructive feedback loop. Treating gum recession is not just about saving teeth--it is about protecting your overall health. For more on this connection, read our article on gum health and heart health.
Book Your Gum Health Evaluation in Marlborough
Regular dental cleanings at Innova Smiles include recession measurement at every visit. If it has been more than 6 months since your last professional cleaning, or if you have noticed any of the warning signs above, schedule an evaluation. Early detection gives you the most treatment options and the best outcomes.
We are located at 340 Maple St, Suite 100, Marlborough, MA 01752. Call (508) 481-0110 or book now. We serve patients throughout MetroWest MA including Framingham, Northborough, Southborough, Shrewsbury, Westborough, and beyond.
Related Articles
- Deep Cleaning vs. Regular Cleaning: Understanding SRP
- The Connection Between Gum Health and Heart Health
- Essential Dental Hygiene Tips for a Healthy Smile
- The 4 Stages of Gum Disease: Early Signs, Risks, and Treatment
- Why Are My Teeth So Sensitive? Causes and Treatments
Related Services
Sources & Further Reading
- Gum Disease & Gum Recession — Health Information — National Institute of Dental and Craniofacial Research (NIH)
- Gum Graft Surgery — Treatments and Procedures — American Academy of Periodontology
- Toothbrushes — Choosing the Right Bristles — American Dental Association (MouthHealthy)
- Chambrone & Tatakis — Periodontal Soft Tissue Root Coverage Procedures (systematic review of graft outcomes) — Cochrane Database of Systematic Reviews
- Journal of Periodontology — American Academy of Periodontology / Wiley