Featured Answer: What Are the Stages of Gum Disease?
Gum disease progresses through four distinct stages, from gingivitis (fully reversible) to advanced periodontitis (which can cause permanent bone loss and tooth loss). The earlier the disease is caught, the simpler, less expensive, and more effective treatment is. At Innova Smiles in Marlborough, MA, Dr. Fatima measures gum pocket depths at every cleaning and exam to detect disease before it advances.
Why Gum Disease Is a Silent Epidemic
Periodontal disease earns its reputation as a "silent" condition because early stages are frequently asymptomatic. Patients feel nothing unusual while bacterial infection systematically destroys the tissue and bone that hold their teeth in place. According to the CDC, 47.2% of adults aged 30 and older, and 70.1% of adults 65 and older, have some form of periodontal disease. Despite these numbers, many people remain undiagnosed until the disease has already caused irreversible structural damage.
Understanding what happens at each stage helps you recognize warning signs early and seek care before problems become severe.
Stage 1: Gingivitis
Reversible with professional treatment and improved home care
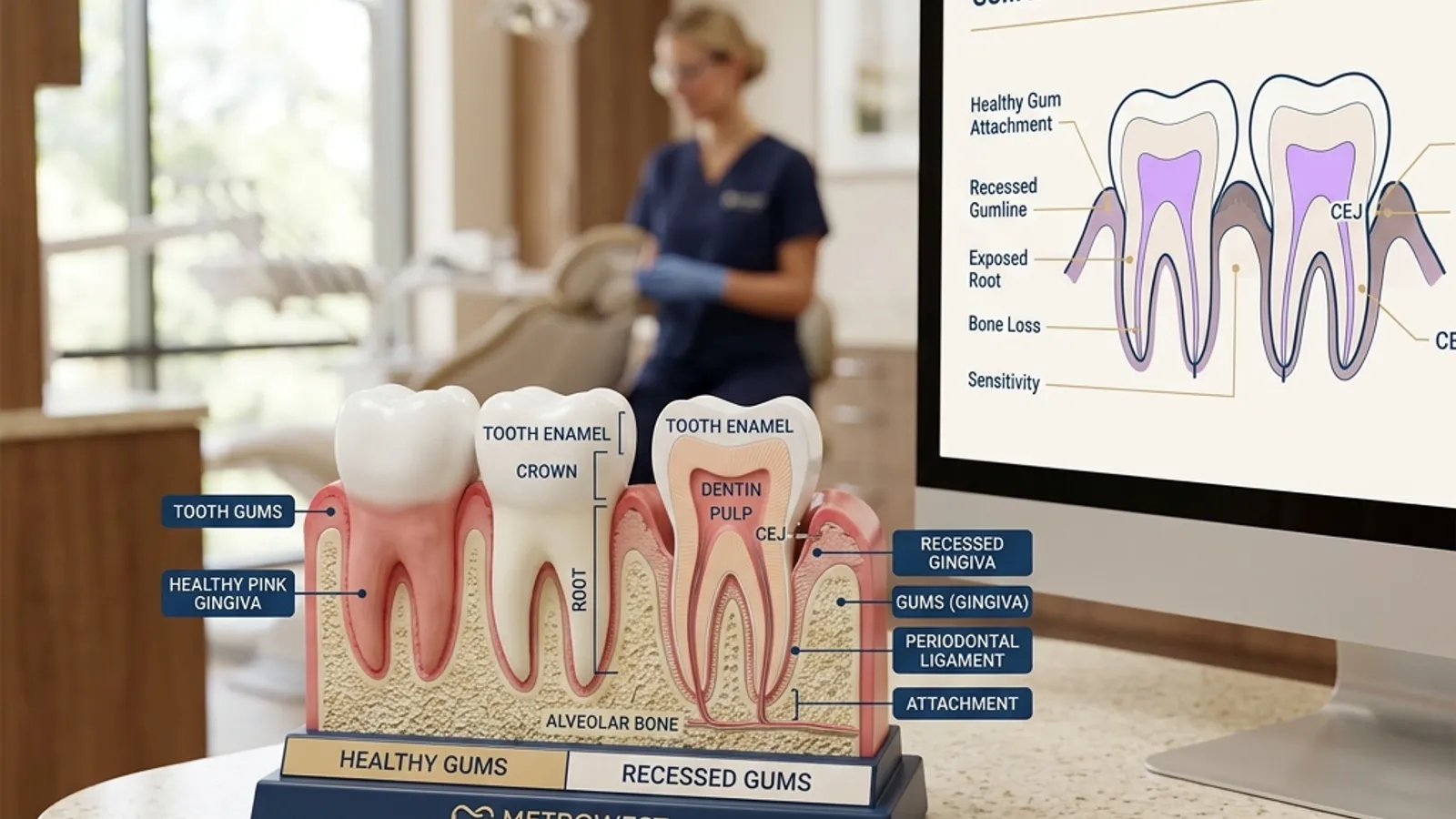
Gingivitis is inflammation of the gum tissue (gingiva) caused by bacterial plaque that has accumulated along and below the gumline. It is the earliest stage of gum disease and the only one that is completely reversible.
Symptoms at Stage 1:
- Gums that bleed during brushing or flossing, the most common and earliest warning sign
- Red, swollen, or puffy gum tissue (healthy gums are pink and firm)
- Gums that feel tender to the touch
- Persistent bad breath that doesn't improve with brushing
- No pain (which is why many patients ignore it)
What is happening clinically: Plaque, the sticky film of bacteria that forms on teeth, produces toxins that irritate gum tissue, causing it to become inflamed. Pocket depths remain 1 to 3 millimeters (the healthy range). There is no bone loss at this stage.
Treatment: A thorough professional cleaning (prophylaxis) to remove plaque and tartar from above and just below the gumline, combined with improved brushing and flossing technique at home, is sufficient to resolve gingivitis entirely. Most patients see significant improvement within 2 to 4 weeks of consistent home care.
Key fact: Gingivitis does not automatically progress to periodontitis. With proper care, the disease can be stopped and reversed at this stage. Without treatment, however, it frequently advances.
Stage 2: Early Periodontitis
Damage is permanent, but progression can be stopped
When gingivitis is left untreated, the bacterial infection spreads below the gumline into the deeper structures supporting the tooth. The body's immune response, while attempting to fight the bacteria, also begins to destroy the periodontal ligament and alveolar bone surrounding the tooth roots. This is the transition from gingivitis to periodontitis.
Symptoms at Stage 2:
- Pocket depths of 4 to 5 millimeters (detectable only with a periodontal probe during an exam)
- Bleeding that is more pronounced and may occur without provocation
- Gums beginning to pull away from teeth, creating visible gaps
- Mild bone loss visible on dental X-rays
- Persistent halitosis despite good hygiene
- Possible early tooth sensitivity as gum tissue recedes
What is happening clinically: Bacteria that produce enzymes capable of breaking down collagen fibers have colonized the periodontal pockets. Early bone loss, typically 1 to 2 millimeters, has occurred around affected teeth. Once bone is lost, it does not regenerate on its own.
Treatment: Scaling and Root Planing (SRP), commonly called a "deep cleaning," is the standard of care. SRP uses specialized ultrasonic and hand instruments to remove bacterial deposits from deep within periodontal pockets, below the gumline. Treatment is completed under local anesthesia, typically over two visits (one per side of the mouth). After SRP, patients transition to periodontal maintenance cleanings every 3 to 4 months rather than the standard 6-month schedule.
Stage 3: Moderate Periodontitis
Significant bone loss; tooth mobility may begin
Moderate periodontitis represents a more advanced stage of the disease with greater bone destruction and increased risk of complications. The infection is deeper and more established, and the structural integrity of affected teeth begins to be genuinely compromised.
Symptoms at Stage 3:
- Pocket depths of 6 to 7 millimeters
- 20% to 50% bone loss around affected teeth (visible on X-rays)
- Teeth that feel slightly loose or have shifted position
- Noticeable gum recession exposing root surfaces
- Increased tooth sensitivity due to root exposure
- Pain when biting or chewing in affected areas
- Abscesses (localized infections) may develop within periodontal pockets
What is happening clinically: The bacterial biofilm has become more complex and harder to eliminate. The infection may have spread to multiple teeth. Bone loss is now significant enough to affect tooth stability. Systemic health connections become more pronounced at this stage, research published in the Journal of Clinical Periodontology links moderate to advanced periodontitis with increased risk of cardiovascular disease, poorly controlled diabetes, and adverse pregnancy outcomes.
Treatment: SRP remains part of the treatment protocol, but surgical intervention is frequently required to access and clean pockets that are too deep for non-surgical instruments to reach effectively. Periodontal surgery, including open flap debridement (where the gum tissue is folded back to allow direct access to roots and bone), is often indicated. Bone grafting procedures may be used to attempt to regenerate lost bone support.
Stage 4: Advanced Periodontitis
Severe bone loss; tooth loss is likely without aggressive intervention
Advanced periodontitis is the most severe form of the disease. More than 50% of bone support has been lost around affected teeth, causing significant mobility, bite changes, and in many cases requiring tooth extraction.
Symptoms at Stage 4:
- Pocket depths greater than 8 millimeters
- Teeth that are visibly loose, shifting, or have changed position (bite feels different)
- Significant spaces developing between teeth (drifting)
- Severe gum recession with extensive root exposure
- Chewing is difficult or painful
- Tooth loss has already occurred or is imminent
- Recurrent abscesses
- Halitosis that is constant and severe
What is happening clinically: The infection has progressed to the point where the structural support for multiple teeth is critically compromised. The periodontal ligament, which anchors the tooth within the jawbone, has been destroyed over a significant portion of the tooth's root surface.
Treatment: Advanced periodontitis typically requires a combination of surgical procedures including osseous surgery (reshaping of the bone to eliminate deep pockets), bone and tissue grafting, and in many cases strategic tooth extractions followed by restorative options such as dental implants or bridges to replace lost teeth. Long-term periodontal maintenance (every 3 months) is essential to prevent recurrence.
Stage Comparison at a Glance
| Stage | Pocket Depth | Bone Loss | Reversible | Treatment |
|---|---|---|---|---|
| Stage 1: Gingivitis | 1–3 mm | None | Yes, fully | Professional cleaning + home care |
| Stage 2: Early Periodontitis | 4–5 mm | Mild (1–2 mm) | No, but stoppable | Scaling and Root Planing (SRP) |
| Stage 3: Moderate Periodontitis | 6–7 mm | 20–50% | No | SRP + periodontal surgery |
| Stage 4: Advanced Periodontitis | 8+ mm | 50%+ | No | Surgery + possible tooth replacement |
Risk Factors That Accelerate Gum Disease
Certain factors make the disease progress faster and more aggressively:
- Smoking and tobacco use: The CDC reports that smokers are 2 to 7 times more likely to develop periodontal disease than non-smokers. Smoking also masks bleeding, an early warning sign, by constricting blood vessels in the gums.
- Diabetes: Poorly controlled blood sugar impairs the immune system's ability to fight infection. The relationship is bidirectional, gum disease also makes blood sugar harder to control.
- Genetics: Some individuals are genetically predisposed to more aggressive forms of the disease regardless of their home care routine.
- Stress: Chronic stress suppresses immune function and increases cortisol levels, which promotes inflammation.
- Medications: Certain blood pressure medications, antidepressants, and immunosuppressants can affect gum tissue health.
- Pregnancy: Hormonal changes during pregnancy increase susceptibility to gum inflammation (pregnancy gingivitis).
The Gum Disease and Systemic Health Connection
Periodontal disease does not exist in isolation. Over the past two decades, an extensive body of research has demonstrated that the chronic inflammation and bacterial burden associated with gum disease affect organ systems throughout the body.
Cardiovascular disease: A 2019 meta-analysis published in the Journal of Clinical Periodontology analyzing data from over 7 million participants found that individuals with periodontitis had a 1.2 to 3.0 times higher risk of coronary heart disease and stroke compared to periodontally healthy individuals, even after adjusting for smoking, diabetes, and hypertension. The proposed mechanism involves both chronic systemic inflammation (elevated CRP and IL-6 levels) and the direct translocation of oral pathogens, particularly Porphyromonas gingivalis, into atherosclerotic plaques.
Diabetes: The relationship between periodontitis and diabetes is bidirectional. Poorly controlled blood sugar impairs immune function in gum tissue, making periodontitis progress faster. Conversely, active gum disease releases inflammatory mediators that worsen insulin resistance. A 2020 Cochrane review found that periodontal treatment (scaling and root planing) produced a statistically significant 0.29% reduction in HbA1c levels at three to four months, a clinically meaningful improvement that supplements medical diabetes management.
Pregnancy outcomes: Research published in Obstetrics & Gynecology has linked moderate to severe periodontitis with a 2.0 to 2.7 times higher risk of preterm birth and low birth weight. The American College of Obstetricians and Gynecologists recommends routine dental care throughout pregnancy, and periodontal treatment during the second trimester is both safe and beneficial.
Respiratory disease: Bacterial pathogens from periodontal pockets can be aspirated into the lungs, particularly in elderly or immunocompromised patients. Research published in the Journal of Clinical Periodontology has established that patients with moderate to severe periodontitis have a significantly elevated risk of pneumonia, with meta-analyses showing approximately 3-fold higher odds of developing pneumonia compared to those with healthy gums, with the proposed mechanism involving aspiration of oral pathogens.
For MetroWest patients managing any of these conditions, maintaining periodontal health at Innova Smiles is not just about saving teeth, it is about supporting whole-body wellness.
Why Routine Dental Exams Catch Gum Disease Early
The most important tool for catching gum disease in its early, reversible stages is a dental exam with periodontal probing, a quick, comfortable measurement of the space between the gum and tooth at six points around every tooth. Combined with dental X-rays that reveal bone levels, this assessment allows Dr. Fatima to identify even Stage 1 and early Stage 2 disease before you have any noticeable symptoms.
Many patients who discover they have early periodontitis are completely surprised, they felt nothing. This is exactly why the American Dental Association recommends exams and cleanings every 6 months.
Frequently Asked Questions About Gum Disease
Q: Can gum disease be cured, or only managed? Gingivitis (Stage 1) can be completely cured with professional cleaning and improved home care, the gum tissue returns to full health with no lasting damage. Once bone loss has occurred (Stages 2 through 4), the disease cannot be "cured" in the sense of restoring lost bone, but it can be arrested and managed indefinitely with proper treatment and consistent periodontal maintenance. Regenerative procedures including bone grafting can restore some lost support in select cases, but prevention and early intervention remain far more effective than surgical correction.
Q: How do I know if I have gum disease if there is no pain? The only reliable way to detect early gum disease is through a professional periodontal evaluation. During your exam at Innova Smiles, your hygienist measures pocket depths at six points around every tooth and checks for bleeding on probing. These measurements reveal disease that is invisible and produces no early symptoms. At-home warning signs include gums that bleed during brushing, persistent bad breath, and gums that appear red or swollen rather than pink and firm.
Q: My parent lost all their teeth to gum disease. Am I at higher risk? Genetic predisposition is a well-established risk factor for periodontal disease. A 2017 genome-wide association study published in Nature Genetics identified multiple gene variants associated with aggressive periodontitis and heightened inflammatory response to oral bacteria. If you have a family history of early tooth loss or severe gum disease, more frequent professional cleanings (every three to four months rather than six) and vigilant home care are especially important.
Schedule a Gum Health Evaluation in Marlborough
If you have noticed any of the warning signs described above, bleeding gums, bad breath that will not go away, or gums that look longer than they used to, do not wait for your next scheduled visit. Early intervention can prevent years of disease progression and spare you from complex, costly treatment.
Innova Smiles is located at 340 Maple St, Suite 100, Marlborough, MA 01752, serving patients from Hudson, Framingham, Northborough, Southborough, Shrewsbury, Westborough, and Sudbury. Call (508) 481-0110 or request an evaluation online.
Questions about your gum health? Call (508) 481-0110 or book a periodontal evaluation.
Related Articles
- Deep Cleaning vs. Regular Cleaning: Understanding SRP
- Gum Recession: Causes, Signs, and Treatment
- The Connection Between Gum Health and Heart Health
Related Services
- Gum Disease Treatment
- Dental Exams & Cleanings
- Preventive Dentistry
- Dental Implants -- when advanced gum disease has caused tooth loss, implants restore full function
Sources & Further Reading
- Periodontal (Gum) Disease — Prevalence & Risk Factors — Centers for Disease Control and Prevention
- Gum Disease — Patient Information — American Dental Association (MouthHealthy)
- Periodontitis and Atherosclerotic Cardiovascular Disease — Consensus & Meta-analysis — Journal of Clinical Periodontology
- Treatment of Periodontal Disease for Glycaemic Control in People with Diabetes Mellitus (review) — Cochrane Database of Systematic Reviews
- Pregnancy and Oral Health Facts — Centers for Disease Control and Prevention (CDC)