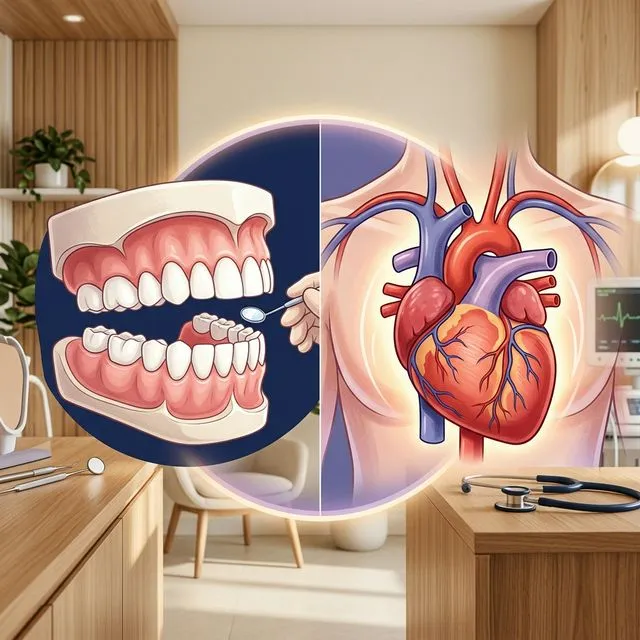
Featured Answer: Can gum disease increase my risk of heart disease?
Yes. A growing body of research — including large-scale epidemiological studies, molecular analyses, and position statements from the American Heart Association — indicates that chronic periodontal disease is independently associated with an increased risk of cardiovascular events. The connection is driven by two primary mechanisms: systemic inflammation triggered by oral infection, and the direct translocation of oral bacteria into the bloodstream where they can contribute to arterial plaque formation.
For decades, medicine treated the mouth as a separate compartment from the rest of the body. That approach is collapsing. At Innova Smiles in Marlborough, Dr. Ambereen Fatima integrates periodontal screening into every examination because the evidence is now clear: what happens in your gums does not stay in your gums.
The Scale of the Problem
Cardiovascular disease remains the leading cause of death in the United States, responsible for approximately 700,000 deaths annually according to the Centers for Disease Control and Prevention (CDC). Periodontal disease, meanwhile, affects nearly half of American adults over age 30, with the prevalence rising to over 70% in adults over 65, per data from the National Institute of Dental and Craniofacial Research (NIDCR).
The overlap between these two conditions is substantial. A landmark 2019 meta-analysis published in the Journal of Clinical Periodontology — examining data from over 7 million participants — concluded that individuals with periodontitis had a 1.2 to 3.0 times higher risk of coronary heart disease, stroke, and peripheral arterial disease compared to periodontally healthy individuals, even after adjusting for traditional cardiovascular risk factors like smoking, diabetes, and hypertension.
Understanding the Inflammation Pathway
The most well-established mechanism linking periodontal disease to cardiovascular disease is chronic systemic inflammation. Here is how it works at the biological level:
The Oral Inflammatory Cascade
Periodontal disease begins when bacterial biofilm (plaque) accumulates along and beneath the gumline. The immune system responds by releasing pro-inflammatory cytokines — signaling molecules including interleukin-1 (IL-1), interleukin-6 (IL-6), and tumor necrosis factor-alpha (TNF-alpha). In health, this response is proportionate and resolves. In periodontitis, the bacterial challenge is persistent, and the inflammatory response becomes chronic.
From Local to Systemic
The inflamed periodontal pocket — the space between the tooth and the gum — acts as a reservoir of chronic infection. The total surface area of ulcerated pocket epithelium in a patient with moderate periodontitis can reach 8–20 square centimeters, roughly the size of the palm of your hand. Through this ulcerated tissue, inflammatory mediators and bacteria gain direct access to the bloodstream.
Once in the blood, these inflammatory molecules improve systemic markers. C-reactive protein (CRP), a well-established cardiovascular risk marker, is significantly improved in patients with periodontal disease. A 2020 study in Hypertension (an American Heart Association journal) found that periodontitis was associated with a 22% higher odds of having improved CRP levels independent of other risk factors.
Endothelial Dysfunction
Chronic low-grade inflammation damages the endothelium — the inner lining of blood vessels. Endothelial dysfunction is one of the earliest detectable steps in the development of atherosclerosis (the buildup of fatty plaques in arteries). When the endothelium is inflamed, it becomes more permeable to LDL cholesterol, more prone to plaque accumulation, and less able to regulate blood pressure through nitric oxide production.
A 2021 randomized controlled trial published in the New England Journal of Medicine reported that intensive periodontal treatment improved flow-mediated dilation — a measure of endothelial function — within six months, suggesting that treating gum disease has a direct, measurable benefit on vascular health.
Bacterial Translocation: Oral Bacteria in the Arteries
Beyond the inflammatory pathway, a second mechanism involves the physical migration of oral bacteria into cardiovascular tissues.
Porphyromonas gingivalis and Arterial Plaque
Porphyromonas gingivalis (P. gingivalis) is one of the primary pathogens responsible for chronic periodontitis. This bacterium has been found alive within atherosclerotic plaques removed from patients during carotid endarterectomy (surgical removal of arterial blockages). A 2019 study in the Journal of the American Heart Association detected P. gingivalis DNA in 100% of coronary artery specimens examined from patients undergoing bypass surgery.
P. gingivalis is not a passive passenger. In laboratory models, this bacterium invades endothelial cells, promotes foam cell formation (a hallmark of atherosclerosis), induces platelet aggregation, and activates matrix metalloproteinases that destabilize existing plaques — potentially triggering plaque rupture, which is the precipitating event in most heart attacks and strokes.
Bacteremia Events
Every time an individual with periodontal disease chews food, brushes their teeth, or undergoes dental procedures, transient bacteremia — bacteria entering the bloodstream — occurs. In a healthy mouth, this is clinically insignificant. In a mouth with active periodontitis, the frequency and magnitude of bacteremia events are dramatically higher, providing repeated opportunities for oral bacteria to seed distant cardiovascular sites.
The American Heart Association's Position
In 2012, the American Heart Association (AHA) published a scientific statement in Circulation acknowledging that periodontal disease is associated with atherosclerotic vascular disease independent of known confounders. The AHA stopped short of declaring a causal relationship, noting that association does not equal causation and that confounding factors (smoking, diabetes, socioeconomic status) are difficult to fully eliminate. However, the statement endorsed the promotion of periodontal health as a component of overall cardiovascular risk reduction.
Since then, additional evidence has strengthened the association. A 2022 consensus report from the European Federation of Periodontology and the World Heart Federation stated that periodontitis should be considered a modifiable risk factor for cardiovascular disease, placing it alongside established risks like hypertension, hyperlipidemia, and smoking.
What Patients Can Do: Actionable Steps
Understanding the oral-cardiovascular connection allows you to take concrete steps that benefit both your gums and your heart. Dr. Fatima recommends the following evidence-based strategies for patients throughout the MetroWest region:
1. Commit to Consistent Oral Hygiene
Brushing twice daily with a fluoride toothpaste and flossing once daily reduces bacterial biofilm and prevents the inflammatory cascade before it starts. The ADA recommends brushing for a full two minutes with a soft-bristled brush. Electric toothbrushes with pressure sensors and timers have been shown in multiple clinical trials to remove significantly more plaque than manual brushing.
2. Never Skip Professional Cleanings
Professional dental cleanings remove calculus (hardened plaque) that cannot be removed with a toothbrush at home. For patients with a history of periodontal disease, Dr. Fatima may recommend periodontal maintenance cleanings every 3–4 months rather than the standard six-month interval. A deep cleaning (scaling and root planing) may be necessary to treat existing disease and establish a healthier baseline.
3. Get Screened at Every Visit
At Innova Smiles, periodontal screening is part of every comprehensive exam. We measure pocket depths, evaluate bleeding on probing, and assess attachment levels. These measurements detect disease before you experience symptoms — which is critical, because early periodontal disease is often painless. Patients from Framingham, Westborough, Sudbury, and surrounding communities benefit from this proactive screening.
4. Control Shared Risk Factors
Many risk factors for periodontal disease and cardiovascular disease overlap: smoking, uncontrolled diabetes, poor nutrition, and chronic stress. Quitting smoking is the single most impactful change a patient can make for both oral and cardiovascular health. The CDC reports that within one year of quitting, excess cardiovascular risk drops by 50%, and periodontal treatment outcomes improve substantially.
5. Share Your Medical History
Inform both your dentist and your physician about your complete health picture. If you take blood pressure medication, cholesterol-lowering drugs, blood thinners, or diabetic medications, your dental team needs to know. Conversely, if your dentist diagnoses periodontal disease, your primary care physician should be informed — especially if you have existing cardiovascular risk factors.
6. Consider a Cardiovascular Risk Assessment
If you have been diagnosed with moderate to severe periodontal disease, it may be worth discussing a cardiovascular risk assessment with your physician. Simple blood tests for CRP, lipid panels, and hemoglobin A1c can provide a more complete picture of your systemic health.
The Importance of Regular Cleanings: Beyond the Surface
Professional cleanings are not simply cosmetic. They are a frontline intervention against systemic inflammation. A 2024 study in the Journal of Periodontology demonstrated that patients who adhered to a regular professional cleaning schedule had 24% lower CRP levels and 17% fewer cardiovascular events over a 10-year follow-up period compared to those who received dental care sporadically.
At Innova Smiles, our hygienists use ultrasonic scalers and fine hand instruments to thoroughly debride all subgingival surfaces. For patients with active periodontal disease, we offer gum disease treatment including scaling and root planing, localized antibiotic therapy, and customized home-care protocols.
Ongoing Research: What's Next
The oral-cardiovascular connection remains one of the most active areas of research in both dentistry and cardiology. Current investigations include:
- Interventional trials — Researchers are conducting randomized controlled trials to determine whether aggressive periodontal treatment reduces the incidence of first and recurrent cardiovascular events.
- Microbiome analysis — Advanced metagenomic sequencing is mapping the specific oral bacterial species most closely associated with cardiovascular pathology.
- Biomarker development — Scientists are working to identify salivary biomarkers that could serve as inexpensive, non-invasive screening tools for cardiovascular risk.
- Vaccine development — Early-stage research is exploring the feasibility of a vaccine against P. gingivalis, which could simultaneously reduce periodontal and cardiovascular disease burden.
While we await the results of these studies, the existing evidence is compelling enough to warrant action. Maintaining excellent oral health is, at minimum, an inexpensive, low-risk strategy with plausible cardiovascular benefit — and undeniable oral health benefit.
Frequently Asked Questions About Oral Health and Heart Disease
Q: If I treat my gum disease, will it lower my heart attack risk? The evidence is promising. A 2021 randomized controlled trial published in the New England Journal of Medicine demonstrated that intensive periodontal treatment improved endothelial function — a measure of vascular health — within six months. A separate 2024 study in the Journal of Periodontology showed that patients who adhered to regular professional cleanings had 17% fewer cardiovascular events over a 10-year period. While no study has yet proven that periodontal treatment directly prevents heart attacks (a causation claim), the reduction in systemic inflammation markers is well established and aligns with what cardiologists target when prescribing statins and anti-inflammatory agents.
Q: Does gum disease cause heart disease, or are they just linked by shared risk factors? This is one of the most debated questions in oral-systemic medicine. Smoking, diabetes, poor diet, and socioeconomic status are risk factors for both conditions, making it difficult to establish direct causation. However, the European Federation of Periodontology and the World Heart Federation issued a joint consensus statement in 2022 classifying periodontitis as a modifiable risk factor for cardiovascular disease — a designation based on interventional studies showing that periodontal treatment measurably reduces CRP and improves endothelial function independent of other risk factor management.
Q: How often should I get cleanings if I have both gum disease and heart disease? Dr. Fatima recommends periodontal maintenance cleanings every three months for patients with active or previously treated periodontitis who also have cardiovascular risk factors. This frequency is supported by research showing that the bacterial biofilm in periodontal pockets reforms to pathogenic levels within 8 to 12 weeks after professional debridement. Quarterly cleanings keep the bacterial challenge below the threshold that triggers chronic inflammation.
Q: Should I tell my cardiologist about my gum disease? Yes. The AHA's 2012 scientific statement in Circulation explicitly recommended that healthcare providers inform patients about the association between periodontal disease and cardiovascular risk. Your cardiologist may factor your periodontal status into risk assessment and may recommend more aggressive management of shared risk factors. Similarly, if your cardiologist has prescribed blood thinners (warfarin, apixaban, clopidogrel), Dr. Fatima needs to know before scheduling deep cleanings or any surgical procedures — dosing adjustments may be necessary.
How Dr. Fatima Approaches the Oral-Systemic Connection
At Innova Smiles, we do not treat teeth in isolation. Dr. Fatima reviews every patient's medical history, medication list, and systemic health conditions as part of the comprehensive exam. If we identify signs of periodontal disease, we explain the systemic implications clearly and collaborate with your physician when appropriate.
Patients from Hopkinton, Northborough, Shrewsbury, and the broader MetroWest area choose Innova Smiles because we practice whole-person dentistry — care that recognizes the mouth is not separate from the body, and that excellent oral health is foundational to overall wellness.
Your gums and your heart are more connected than you might think. Call (508) 481-0110 or schedule your periodontal screening today.
Related Articles
- Deep Cleaning vs. Regular Cleaning: Understanding SRP
- Oral Health and Overall Wellness
- Diabetes and Your Teeth: The Oral Health Connection
- The 4 Stages of Gum Disease: Early Signs, Risks, and Treatment
Related Services
- Gum Disease Treatment (Periodontal Therapy) -- scaling, root planing, and advanced periodontal care
- Dental Exams & Cleanings -- comprehensive exams with full periodontal screening
- Preventive Dentistry -- proactive care to stop gum disease before it starts