Featured Answer: Are implants permanent?
With healthy gums, good home care, and professional maintenance, dental implants often last decades, and the titanium post itself can last a lifetime. Success starts with precise planning and placement by a credentialed implant dentist and continues with daily hygiene and routine checkups to prevent peri-implant disease.
For patients in Marlborough, MA and throughout MetroWest, dental implants represent one of the most reliable long-term investments in oral health. At Innova Smiles, Dr. Ambereen Fatima (FICOI, FAAIP) places every implant with longevity as a primary goal, using CBCT-guided planning and evidence-based protocols to maximize the lifespan of your restoration.
How Long Do Dental Implants Actually Last? The Data by Decade
The short answer: the titanium post is designed to last a lifetime. The crown or prosthesis on top typically lasts 15 to 25 years. But the details matter, so here is what the published research actually shows at each time horizon.
10-Year Survival and Success Rates
A comprehensive systematic review published in the Journal of Dental Research (2012, Pjetursson et al.) analyzed data from 23 prospective and retrospective studies and found:
- Implant survival rate: 95.2% at 10 years (meaning the implant remained in the jaw)
- Implant success rate: 89.7% at 10 years (meaning the implant had no complications, no bone loss exceeding 1.5 mm, no soft tissue problems, full function)
The distinction between survival and success matters. An implant may survive (remain in the jaw) but still develop complications like progressive bone loss or gum recession. True long-term success means the implant remains stable, the surrounding tissues stay healthy, and the restoration continues to function and look natural.
20-Year Data
A 2019 study in Clinical Oral Implants Research (Raikar et al.) tracking implants placed over two decades reported:
- Cumulative survival rate: 92.8% at 20 years
- The most common reason for late failure was peri-implantitis (the implant equivalent of gum disease), accounting for roughly 65% of late implant losses
30+ Year Data
Long-term follow-up data from Professor Branemark's original patients in Sweden, the first humans to receive modern titanium implants in the 1960s, showed implants still functioning after 30 to 40 years. A 2019 retrospective analysis published in the International Journal of Oral & Maxillofacial Implants reported functional implants at 34 years post-placement with stable bone levels in patients who maintained regular professional care.
What About the Crown?
The implant crown (the visible tooth) is a separate component from the titanium post. Implant crowns are typically made from porcelain fused to zirconia or monolithic zirconia. A 2018 systematic review in the Journal of Prosthetic Dentistry found:
- Porcelain-fused-to-metal crowns: 93.4% survival at 10 years
- All-ceramic/zirconia crowns: 95.6% survival at 10 years
- Average crown replacement occurs at 15 to 25 years due to normal wear, chipping, or aesthetic changes
Replacing a crown on an existing, healthy implant is a straightforward procedure, it does not require surgery. The original implant post stays in place.
The Cost-Per-Year Analysis: Why Implants Are the Best Value
A single dental implant costs $3,000 to $6,000 including the crown. That sounds significant until you calculate the cost per year of service compared to alternatives.
| Replacement Option | Average Cost | Average Lifespan | Cost Per Year |
|---|---|---|---|
| Dental implant | $4,500 | 25+ years | $180/year |
| Fixed bridge | $3,500 | 10–15 years | $233–$350/year |
| Removable partial denture | $1,800 | 5–8 years | $225–$360/year |
The implant also preserves the adjacent teeth (a bridge requires grinding down two healthy teeth) and prevents bone loss in the jaw. When you factor in the cost of replacing bridges and partials multiple times over a lifetime, the implant is typically the most economical choice by age 65 to 70.
For MetroWest patients comparing options, we provide detailed cost breakdowns during the consultation. We also work with major insurance carriers and offer financing through our in-house membership plan and third-party options.
Factors That Affect How Long Your Implant Lasts
Not every implant will last 30 years. Certain factors significantly influence longevity, and understanding them helps you protect your investment.
Factors You Can Control
- Oral hygiene: This is the single most important factor. Patients who brush twice daily, use interdental tools around the implant, and attend regular professional cleanings have dramatically better outcomes than those who do not
- Smoking: A 2019 meta-analysis in the Journal of Oral & Maxillofacial Surgery found that smokers had an implant failure rate 2.3 times higher than non-smokers. Smoking impairs blood flow to the bone and gum tissue, slows healing, and promotes bacterial infection. If you smoke, quitting before implant placement is one of the most impactful things you can do for your outcome
- Bruxism management: Chronic teeth grinding places excessive lateral forces on implants that the titanium-bone interface is not designed to handle. A custom night guard is essential for implant patients who grind
- Regular professional maintenance: Implants that receive consistent professional care have measurably better survival rates than those that do not. A 2020 study in the Journal of Clinical Periodontology found that patients who attended maintenance visits at least twice per year had a 90% lower risk of peri-implantitis compared to those who did not
Factors Related to Placement Quality
- Implant position: An implant placed at the wrong angle or depth will experience uneven force distribution, accelerating bone loss
- Bone quality and quantity: Placing an implant into insufficient bone without grafting first compromises the foundation
- Prosthetic design: A crown or bridge that does not allow the patient to clean effectively around the implant sets the stage for peri-implantitis
- Clinician experience: The Journal of Oral Implantology published data showing that implant success rates improve with surgeon experience, with fellowship-trained implant dentists reporting some of the highest long-term success rates
Dr. Fatima's FICOI (Fellow of the International Congress of Oral Implantologists) and FAAIP (Fellow of the American Academy of Implant Prosthodontics) credentials represent hundreds of hours of post-doctoral implant training focused specifically on surgical technique, prosthetic design, and complication management. Read more about why implant credentials matter.
Systemic Health Factors
- Uncontrolled diabetes: Elevated blood sugar impairs osseointegration and increases infection risk. Patients with well-controlled diabetes (HbA1c below 7%) have implant success rates comparable to non-diabetic patients
- Osteoporosis: While osteoporosis alone is not a contraindication for implants, patients taking bisphosphonate medications (Fosamax, Boniva) require careful evaluation due to the rare risk of osteonecrosis
- Autoimmune conditions: Conditions requiring immunosuppressive medications may slow healing, though implants remain a viable option with proper planning
- Radiation therapy to the jaw: Prior radiation can compromise bone vascularity. Hyperbaric oxygen therapy may be recommended before implant placement in irradiated patients
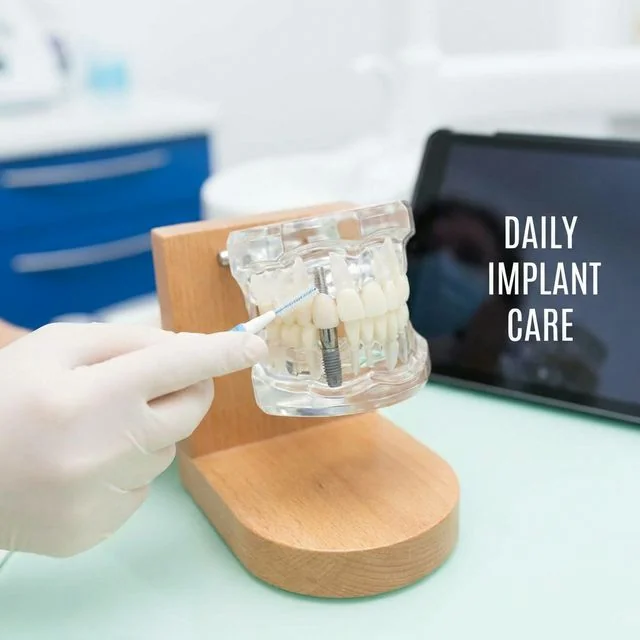
Your Daily Maintenance Routine
Caring for implants at home is straightforward, but consistency matters. Follow this daily protocol:
- Brush twice daily with a soft-bristle or electric toothbrush, angling the bristles toward the gumline around the implant. Spend at least 10 seconds on each surface of the implant crown
- Use interdental tools, a water flosser is the most-recommended option for implant maintenance. Set it to medium pressure and direct the stream around the implant collar. Interdental brushes and implant-specific floss (such as SuperFloss) are also effective
- Rinse with an alcohol-free antimicrobial mouthwash to reduce bacterial buildup without drying out oral tissues. Look for products containing cetylpyridinium chloride (CPC)
- Avoid abrasive toothpaste, whitening pastes with harsh abrasives (look for RDA values above 100) can scratch the surface of implant restorations, creating micro-grooves where bacteria accumulate
Patients from Framingham, Sudbury, Southborough, and surrounding communities who follow these habits consistently see the best long-term results.
Professional Maintenance at Innova Smiles
Professional cleanings for implant patients differ from standard cleanings in important ways. At our Marlborough office, we use implant-safe instruments made from titanium, plastic, or carbon fiber to avoid scratching the implant surface. Metal scalers and ultrasonic tips designed for natural teeth can damage the titanium oxide layer that protects the implant surface and promotes tissue attachment.
During each maintenance visit, we:
- Remove calculus and biofilm from around the implant and under the prosthesis using implant-specific curettes and rubber-cup polishing with a non-abrasive paste
- Measure probing depths around the implant at six points to detect early signs of peri-implantitis. Healthy implant probing depths are typically 3 mm or less. Depths increasing over time signal developing problems
- Assess bleeding on probing; while bleeding may indicate early inflammation, a single isolated bleeding site among the six peri-implant probing sites does not necessarily indicate peri-implant disease. We interpret bleeding in context with probing depths greater than 5 mm, radiographic bone loss, and visual signs of inflammation. Multiple bleeding sites or persistent bleeding warrants further investigation and may indicate peri-implant mucositis or peri-implantitis
- Take periodic radiographs to monitor crestal bone levels. We compare each X-ray to baseline images taken at the time of crown delivery to detect even subtle changes
- Check abutment screw tightness, a loose screw causes micro-movement that can lead to bone loss and eventual failure
- Evaluate the crown for wear, chipping, cement washout, or margin breakdown
- Review your home care technique and recommend adjustments if biofilm patterns suggest areas being missed
We recommend implant maintenance visits every six months. Patients with a history of gum disease, diabetes, or smoking may benefit from visits every 3 to 4 months during the first two years after placement.
Understanding Peri-Implantitis: The Primary Threat to Implant Longevity
Peri-implantitis is a destructive inflammatory condition affecting the tissues around dental implants. It is the leading cause of late implant failure, and it progresses faster than periodontitis around natural teeth because implants lack the periodontal ligament fibers that help resist bacterial invasion.
How Common Is Peri-Implantitis?
A 2018 meta-analysis in the Journal of Clinical Periodontology found that peri-implantitis affects approximately 22% of implants and 43% of implant patients at some point. These numbers are higher than many patients expect, which is why preventive maintenance is so critical.
Risk Factors for Peri-Implantitis
- History of periodontal disease (the single strongest predictor)
- Smoking
- Poor oral hygiene
- Diabetes
- Cement-retained crowns (excess cement trapped under the gum is a common trigger)
- Lack of keratinized (firm, attached) gum tissue around the implant
How We Treat Peri-Implantitis
When caught early (peri-implant mucositis, the reversible precursor to peri-implantitis), treatment involves professional debridement, antimicrobial rinses, and improved home care. The condition is fully reversible at this stage.
Once true peri-implantitis develops with bone loss, treatment becomes more involved:
- Mechanical debridement with implant-safe instruments
- Antimicrobial therapy, local delivery of minocycline or chlorhexidine into the peri-implant pocket
- Surgical access and bone grafting for advanced cases — Dr. Fatima opens a flap to decontaminate the implant surface and graft bone material to rebuild lost support
- Surface decontamination using laser therapy or chemical agents to remove the bacterial biofilm from the implant's textured surface
The key message: peri-implantitis is far easier to prevent than to treat. Every dollar spent on maintenance saves many dollars in surgical intervention later.
Signs of Dental Implant Failure
The American Academy of Implant Dentistry reports that while implant failure is rare (occurring in fewer than 5% of cases), recognizing the warning signs early can make the difference between saving and losing an implant.
Early Failure (Within Weeks to Months of Placement)
Early failure happens before the implant fully integrates with the bone. Signs include:
- Implant feels loose or mobile when you press on it with your tongue
- Sharp or throbbing pain at the implant site that does not improve after the normal 7 to 10 day healing window
- Swelling that worsens after the first week rather than improving
- The implant feels like it is sinking or the gum tissue around it is receding rapidly
Common causes of early failure include infection at the surgical site, insufficient bone density, premature loading (placing too much force on the implant before osseointegration is complete), overheating the bone during drilling, and systemic health factors like uncontrolled diabetes or smoking.
Late Failure (Months to Years After Placement)
Late failure occurs after successful osseointegration, usually due to peri-implantitis or mechanical overload. Watch for:
- Bleeding or swelling around the implant that persists despite good oral hygiene
- Looseness or movement in the crown or the implant itself
- A change in your bite when chewing, the implant feels higher or different
- Persistent bad taste or odor near the implant site, indicating bacterial infection
- Gum recession exposing the metal abutment or implant threads
- Bone loss visible on X-rays during routine checkups (you may not feel this)
What to Do If You Suspect Implant Problems
Contact Innova Smiles promptly at (508) 481-0110 if you notice any of the symptoms above. Early intervention is critical. A 2023 study in the Journal of Clinical Periodontology confirmed that peri-implantitis can lead to progressive bone loss and eventual implant failure if left untreated, but that early-stage disease responds well to non-surgical therapy when caught within the first year of onset. Dr. Fatima monitors implant health at every maintenance visit using probing measurements and periodic radiographs to catch issues before they become serious.
The Role of Advanced Technology
Innova Smiles invests in technology that supports implant longevity from day one:
- CBCT 3D scanning enables precise measurement of bone height, width, and density before surgery. This eliminates guesswork and allows Dr. Fatima to select the optimal implant size and position
- Guided surgical protocols use a 3D-printed surgical guide that fits over your teeth and directs the drill to the exact planned position. A 2021 systematic review in Clinical Oral Implants Research found that guided surgery reduced placement errors by 50% compared to freehand techniques
- Digital impressions ensure the crown fits precisely on the implant, eliminating the micro-gaps that can harbor bacteria and lead to peri-implantitis
To learn more about how this technology works, see our guide on guided implant surgery and CBCT precision.
Building Your Implant Maintenance Calendar
Here is a practical schedule to keep your implant healthy for decades:
| Timeline | Action |
|---|---|
| Daily | Brush 2x, water flosser, interdental brushes, antimicrobial rinse |
| Every 6 months | Professional implant cleaning + probing + radiograph review |
| Annually | Comprehensive implant evaluation with CBCT if indicated |
| Every 5 years | Abutment screw torque check and crown integrity assessment |
| Every 15–25 years | Crown replacement due to normal wear |
| Ongoing | Night guard use if you grind, smoking cessation support if needed |
Patients from Hudson, Northborough, Westborough, and throughout MetroWest trust Innova Smiles for both implant placement and the long-term maintenance that protects their investment. Dr. Fatima's dual fellowship training (FICOI and FAAIP) means you receive expert care from placement through every year of follow-up.
Your implant is an investment in decades of function, confidence, and quality of life. Protecting that investment takes 5 minutes of daily care and two professional visits per year. That is a remarkable return.
Protect your investment. Call (508) 481-0110 or book now.
Related Articles
- Dental Implant Recovery: Day-by-Day Timeline
- Types of Dental Implants: Titanium vs. Zirconia
- Why Implant Credentials (FICOI & FAAIP) Matter